Table of contents
- Main points
- Collaboration
- Things you need to know about this release
- All-cancers combined survival index
- Breast, colorectal and lung cancer: one-year survival
- Interpretation of these statistics
- Who uses these statistics and for what purpose?
- Links to other related statistics
- Quality and methodology
- Authors
- Acknowledgements
1. Main points
All-cancers survival index
The one-year all-cancer survival index for England increased steadily from 61.2% for patients diagnosed in 2000 to 72.3% in 2015.
The one-year all-cancer survival index increased steadily in most Clinical Commissioning Groups (CCGs) throughout that period; for patients diagnosed in 2015, the all-cancer survival index for CCGs ranged from 67.0% to 77.4%, compared with 49.5% to 66.6% in 2000.
The inequality gap in the cancer survival index between the highest and lowest CCG in England has shrunk since 2000.
Sustainability and Transformation Partnerships (STPs) have been included in this bulletin for the first time; for patients diagnosed in 2015, the all-cancer survival index for STPs ranged from 70.0% to 75.1%, compared with 55.5% to 65.9% based on data for 2000.
As for CCGs, the inequality gap between the highest and lowest STP in England has reduced since 2000, having halved for STPs over this period.
Survival for breast, colorectal and lung cancer
In 2015, one-year age-standardised breast cancer survival in England was 96.7%, increasing from 92.8% for patients diagnosed in 2000; for all the CCGs, in 2015, the difference between the highest survival estimate (98.8%) and the lowest (92.1%) was 6.7 percentage points.
In England, one-year age-sex-standardised survival for patients diagnosed with colorectal cancer has steadily increased from 72.6% in 2000 to 80.4% in 2015; among the 207 CCGs, the difference between the highest one-year survival estimate in 2015 (85.3%) and the lowest (70.8%) was 14.5 percentage points.
In England, one-year age-sex-standardised survival for patients diagnosed with lung cancer increased from 25.7% in 2000 to 40.7% in 2015; for all the CCGs, in 2015, the difference between the highest survival estimate (55.2%) and the lowest (28.6%) was 26.6 percentage points.
2. Collaboration
The cancer survival data in this bulletin have been collected and calculated by the National Cancer Registration and Analysis Service (NCRAS) within Public Health England (PHE) and published in partnership with Office for National Statistics (ONS).

3. Things you need to know about this release
What’s included in this bulletin?
This bulletin focuses on trends in the one-year survival index for all cancers combined (excluding non-melanoma skin cancer and prostate cancer) for each of the 207 Clinical Commissioning Groups (CCGs), for the 44 Sustainability and Transformation Partnerships, and for England as a whole.
The cancer survival index provides a convenient, single number that summarises the overall pattern of cancer survival. A more detailed definition is provided in Section 6.
Separate one-year survival estimates for breast (women only), colorectal (bowel) and lung cancer are also presented in this bulletin at CCG level. These estimates are age-standardised (breast cancer) or age-sex-standardised (colorectal and lung cancers). Net survival is estimated for adults (aged 15 to 99 years) who were diagnosed with cancer between 2000 and 2015 and followed up to 31 December 2016. Survival is estimated using flexible parametric models. More information on methodology can be found in the Quality and Methodology Information report.
Differences are based on the exact underlying survival estimates, but they are shown in the bulletin at one decimal place.
Although not commented on in the bulletin, the reference tables contain the following extra data for breast (women), colorectal and lung cancer separately, these three cancers combined, and all-cancers (excluding non-melanoma skin cancer and prostate cancer):
five-year and 10-year net cancer survival index for England and the 44 Sustainability and Transformation Partnerships (STPs) in England
separate estimates for the all-cancers combined index and the three-cancers combined index for adults aged 55 to 64 years and 75 to 99 years
mid-year population estimates and the number of cancer patients included in the analysis (Table 4 and 9)
confidence intervals (at the 95% level) and precision estimates for each survival estimate
What’s changed in this release?
As part of this new partnership with Public Health England, the methods were reviewed, which has led to a change in weights based on the International Classification of Survival Standard (ICSS) for age standardisation. Further details of these methodology changes can be found in the Impact of updating cancer survival methodologies for sub-national estimates; Index of cancer survival for Clinical Commissioning Groups, which outlined the minimal differences in these estimates compared with the previous methodology.
How to interpret these statistics
The cancer survival index has been designed specifically to reduce the impact of random variation in the year-on-year cancer-specific estimates due to sparse data. Interpretation should focus on overall trends and the relative position of each CCG in the funnel plots throughout the years, rather than on small changes in the survival index in a particular year.
Data are provided for this 16-year period so that each CCG has a baseline against which to assess progress over time. Survival estimates should not be used as the only indicator of a CCG's performance in cancer outcomes. Furthermore, the statistical models used for these estimates mean that direct comparisons between CCGs for a given year may be unreliable.
A CCG for which the survival index is consistently lower than average should nevertheless be considering why survival in its area might be low, even if it is not identified as an outlier. This is even more crucial when examining the survival estimates for breast, lung and colorectal cancers separately. For more information and guidance on funnel plots, see “Interpreting the survival estimates in this bulletin”.
These cancer survival estimates are designated as National Statistics. National Statistics are a subset of official statistics, which have been certified by the UK Statistics Authority as compliant with its Code of Practice for Official Statistics.
Back to table of contents4. All-cancers combined survival index
One-year survival for all-cancers combined in England increased from 61.2% in 2000 to 72.3% in 2015. The index increased steadily for Clinical Commissioning Groups (CCGs) throughout that period. In 2015, the survival index ranged from 67.0% (NHS Barking and Dagenham CCG, and NHS Medway CCG) to 77.4% (NHS Richmond CCG), compared with 49.5% (NHS Waltham Forest CCG) to 66.6% (NHS Vale of York CCG) in 2000 (Figure 1).
The difference between the highest and lowest values of the one-year survival index for CCGs has decreased, from 17.1% in 2000 to 10.4% in 2015. As a result, the values of the survival index for CCGs cluster more closely around the England average in 2015 than in 2000 (Figure 1). The survival index for every CCG in 2015 is now higher than the overall value for England (61.2%) in 2000.
In general, the largest increases between 2000 and 2015 were in areas where survival was lower in 2000. For example, one-year survival in NHS Waltham Forest CCG (lowest estimate in 2000) increased by 20.9 percentage points between 2000 and 2015, and by 5.0 percentage points in NHS Vale of York CCG (highest estimate in 2000).
Figure 1: Funnel plot of the one-year survival index (%) for all cancers combined, for Clinical Commissioning Groups (CCG): England
Adults (aged 15 to 99 years) diagnosed in 2000 and in 2015
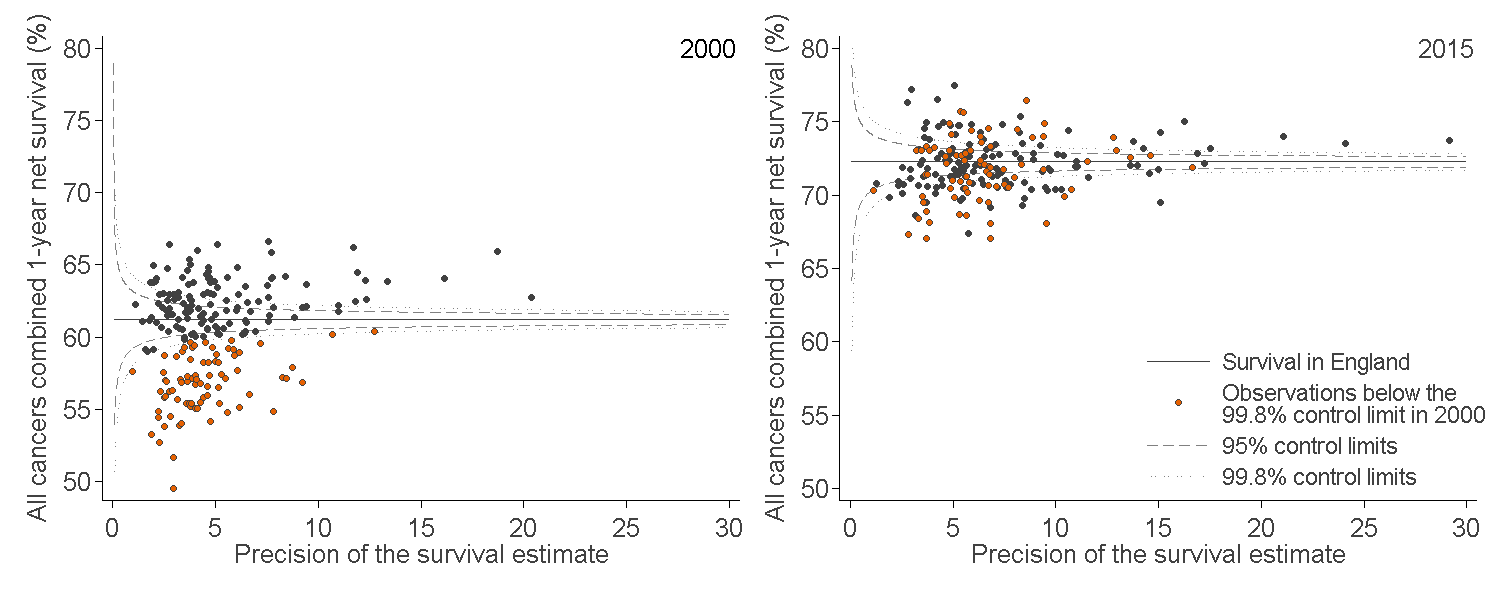
Source: National Cancer Registration and Analysis Service within Public Health England; Office for National Statistics
Notes:
Each data point represents a single CCG. The higher the precision, the more reliable the survival estimate. More information on how to interpret these funnel plots can be found in the “How to interpret a funnel plot” section.
The survival estimates identified as “outliers” fell above or below the 99.8% control limits (the wider of the two “funnels” around the England estimate) at each level of precision.
Download this image Figure 1: Funnel plot of the one-year survival index (%) for all cancers combined, for Clinical Commissioning Groups (CCG): England
.png (73.4 kB) .xls (60.9 kB)A persistent feature of these data is that the one-year survival index is generally lower in the north of England than in the south. In 2015, of the 59 CCGs where the one-year index is significantly below the England average, 27 (45.8%) were in the North of England and 17 (28.8%) were in the Midlands and East of England.
By contrast, 19 (42.2%) of the 45 CCGs where the one-year index is significantly above the England average were in the South of England (Figure 2). This was closely followed by London, which had one-third (15 CCGs) of CCGs with survival estimates significantly higher than the England average.
Figure 2: Map of the one-year survival index for all cancers combined compared with the England average, for Clinical Commissioning Groups (CCG)
Adults (aged 15 to 99 years) diagnosed in 2015
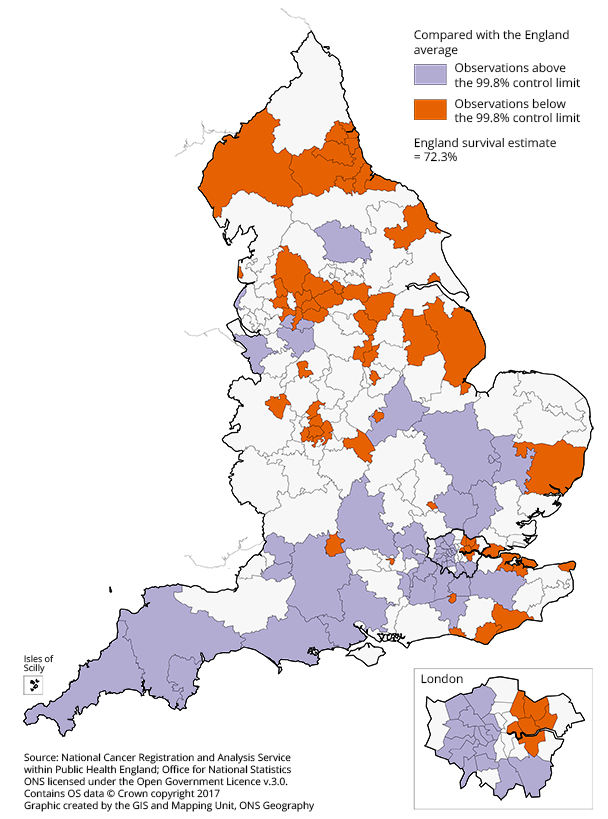
Download this image Figure 2: Map of the one-year survival index for all cancers combined compared with the England average, for Clinical Commissioning Groups (CCG)
.png (248.5 kB) .xls (52.7 kB)The index increased steadily for the areas now defined by the Sustainability and Transformation Partnerships (STPs) throughout the period 2000 to 2015. In 2015, the survival index ranged from 70.0% (for both The Black Country and North East London) to 75.1% (Surrey Heartlands), compared with 55.5% (North East London) to 65.9% (Dorset) in 2000. The inequality gap between the highest and lowest STP in England has halved since 2000, from 10.4 to 5.1 percentage points. As expected, the range in survival estimates between STPs is smaller than the range between CCGs in England.
For 2015, the highest CCG survival estimate was in NHS Richmond CCG, which is within the South West London STP; however, the highest STP estimate was Surrey Heartlands. In contrast, the lowest CCG estimate was NHS Barking and Dagenham CCG, which is within the North East London STP; this was also the STP with the lowest survival estimate.
Back to table of contents5. Breast, colorectal and lung cancer: one-year survival
Estimates of one-year age-standardised survival for breast cancer (women) and age-sex-standardised survival for colorectal and lung cancer in each Clinical Commissioning Group (CCG) and Sustainability and Transformation Partnership (STP) are also presented in this bulletin. Funnel plots of CCG estimates for 2000 and 2015 are presented in the commentary for comparison.
We provide a guide to interpreting these survival estimates and funnel plots in the section “Interpretation of these statistics”.
One-year age-standardised breast cancer survival
In 2015, one-year breast cancer survival in England was 96.7%, increasing from 92.8% for patients in 2000. Figure 3 shows a very tight clustering in survival in 2015 for CCGs around the England average compared with 2000: the difference between the highest survival estimate (98.8% in NHS West London CCG) and the lowest (92.1% in NHS South Tyneside CCG) in 2015 was 6.7 percentage points.
Figure 3: Funnel plot of the one-year age-standardised survival (%) for breast cancer, for Clinical Commissioning Groups (CCG)
England, women (aged 15 to 99 years) diagnosed in 2000 and in 2015
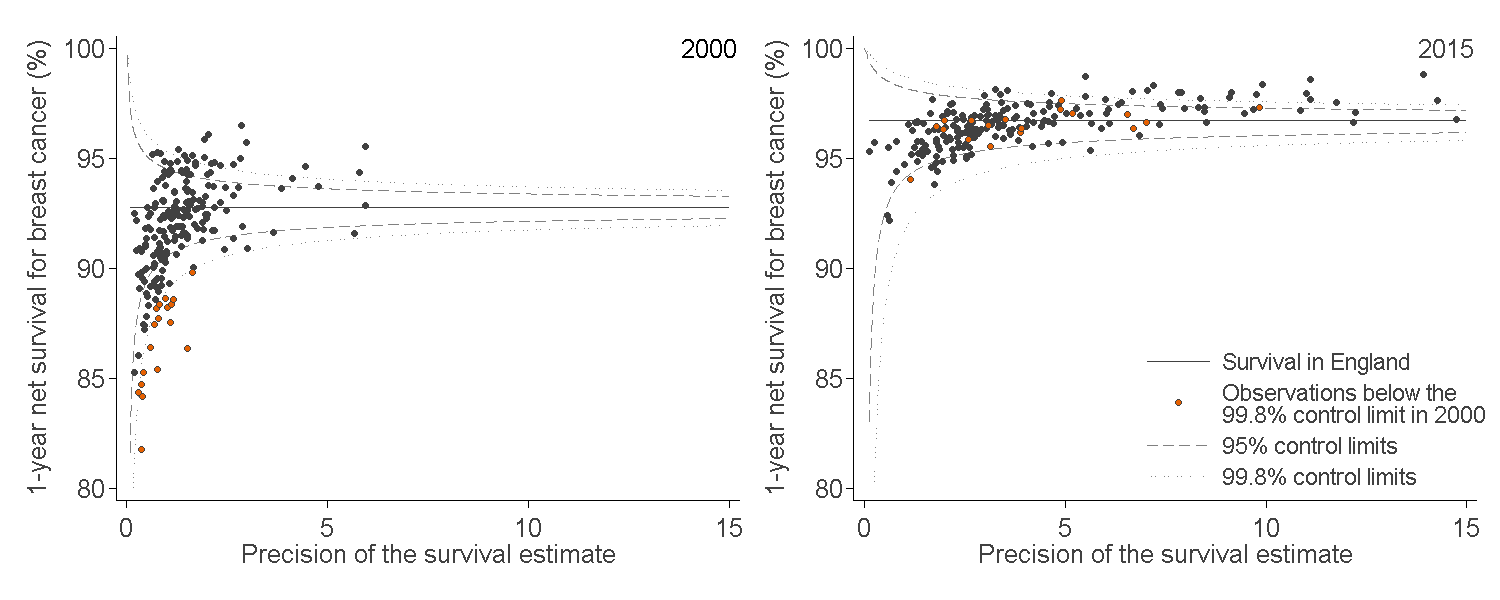
Source: National Cancer Registration and Analysis Service within Public Health England; Office for National Statistics
Notes:
Each data point represents a single CCG. The higher the precision, the more reliable the survival estimate. More information on how to interpret these funnel plots can be found in the “How to interpret a funnel plot” section.
The survival estimates identified as “outliers” fell above or below the 99.8% control limits (the wider of the two “funnels” around the England estimate) at each level of precision.
Download this image Figure 3: Funnel plot of the one-year age-standardised survival (%) for breast cancer, for Clinical Commissioning Groups (CCG)
.png (68.1 kB) .xls (81.9 kB)A persistent feature of these data is that one-year breast cancer survival is only significantly lower than the England average in a small number of CCGs. In 2015, these were:
- NHS South Tyneside CCG, at 92.1%
- NHS Swale CCG, at 92.4%
- NHS South Kent Coast CCG, at 93.8%
- NHS Mansfield and Ashfield CCG, at 94.4%
- NHS Birmingham CrossCity CCG, at 95.3%
In 2015, of the 207 CCGs across the country, 15 had a one-year survival index significantly higher than the England average (Figure 4).
Figure 4: Map of the one-year age-standardised survival for breast cancer compared with the England average, for Clinical Commissioning Groups (CCG)
Women (aged 15 to 99 years) diagnosed in 2015
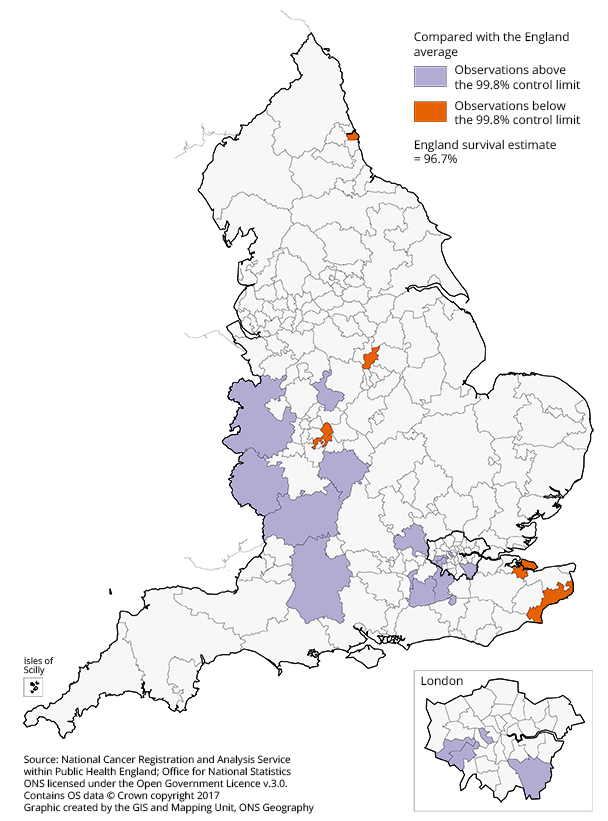
Download this image Figure 4: Map of the one-year age-standardised survival for breast cancer compared with the England average, for Clinical Commissioning Groups (CCG)
.png (234.5 kB) .xls (51.7 kB)For one-year survival in STPs, the difference between the highest estimate (97.9% in Shropshire, and Telford and Wrekin) and the lowest estimate (95.5% in Norfolk and Waveney) for breast cancer was 2.4 percentage points.
One-year age-sex-standardised colorectal cancer survival
In England, one-year survival for patients diagnosed with colorectal cancer has increased steadily from 72.6% in 2000 to 80.4% in 2015. In 2000, the majority of CCGs identified as outliers lower than the England average are now similar to the England average in 2015 (Figure 5).
The range between the highest and lowest estimate of one-year survival for CCGs was 14.5 percentage points in 2015 (85.3% in NHS North East Hampshire and Farnham CCG compared with 70.8% in NHS Leicester City CCG).
Figure 5: Funnel plot of the one-year age-sex-standardised survival (%) for colorectal cancer, for Clinical Commissioning Groups (CCG)
England, adults (aged 15 to 99 years) diagnosed in 2000 and in 2015
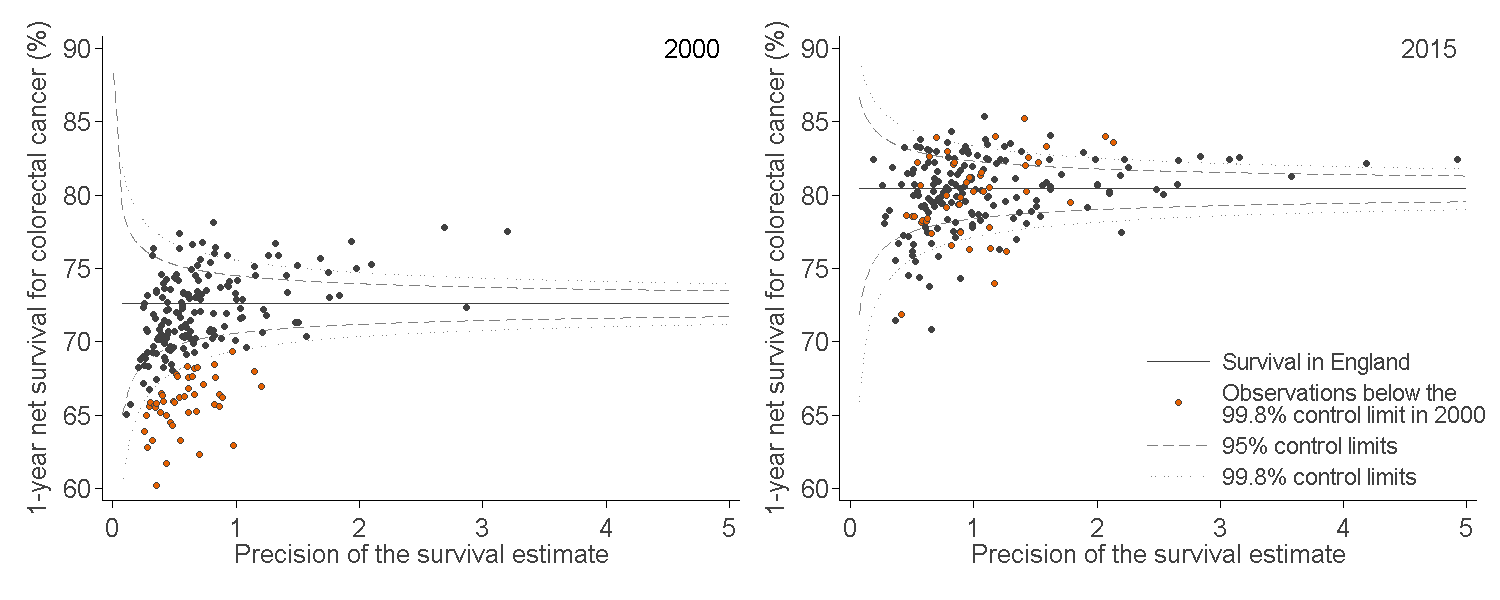
Source: National Cancer Registration and Analysis Service within Public Health England; Office for National Statistics
Notes:
Each data point represents a single CCG. The higher the precision, the more reliable the survival estimate. More information on how to interpret these funnel plots can be found in the “How to interpret a funnel plot” section.
The survival estimates identified as “outliers” fell above or below the 99.8% control limits (the wider of the two “funnels” around the England estimate) at each level of precision.
Download this image Figure 5: Funnel plot of the one-year age-sex-standardised survival (%) for colorectal cancer, for Clinical Commissioning Groups (CCG)
.png (71.0 kB) .xls (83.5 kB)In 2015, there were 19 CCGs across England that had a one-year survival index significantly higher than the national average, whilst 21 CCGs had one-year colorectal cancer survival estimates significantly lower than the England average, as shown in Figure 6.
Figure 6: Map of the one-year age-sex-standardised survival for colorectal cancer compared with the England average, for Clinical Commissioning Groups (CCG)
Adults (aged 15 to 99 years) diagnosed in 2015
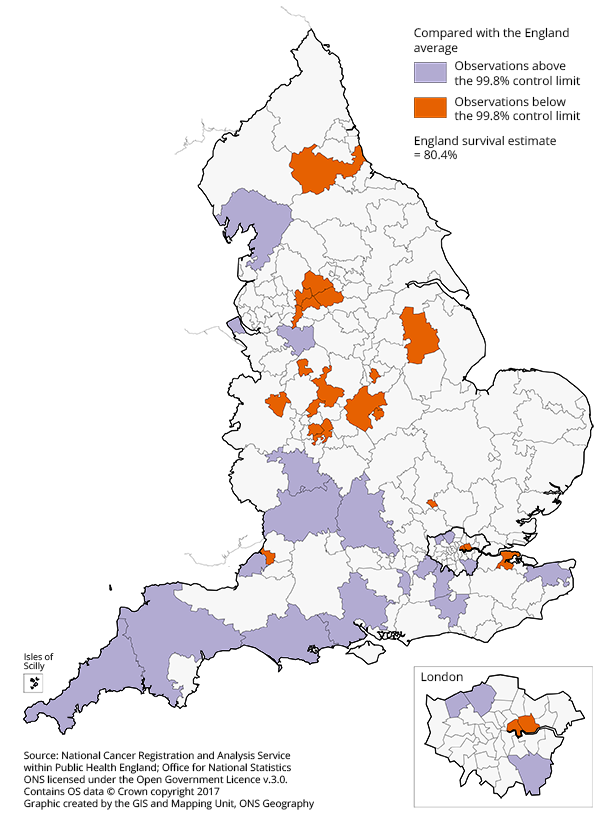
Download this image Figure 6: Map of the one-year age-sex-standardised survival for colorectal cancer compared with the England average, for Clinical Commissioning Groups (CCG)
.png (240.4 kB) .xls (44.5 kB)For one-year survival in STPs, the difference between the highest estimate (83.8% in Surrey Heartlands) and the lowest estimate (76.6% in Leicester, Leicestershire and Rutland) for colorectal cancer was 7.2 percentage points.
One-year age-sex-standardised lung cancer survival
In England, one-year survival for patients diagnosed with lung cancer increased from 25.7% in 2000 to 40.7% in 2015 (Figure 7). The range between the highest and lowest estimate of one-year survival for CCGs was 26.6 percentage points in 2015 (55.2% in NHS Central London (Westminster) CCG compared with 28.6% in NHS Medway CCG).
Figure 7: Funnel plot of the one-year age-sex-standardised survival (%) for lung cancer, for Clinical Commissioning Group (CCG)
England, adults (aged 15 to 99 years) diagnosed in 2000 and in 2015
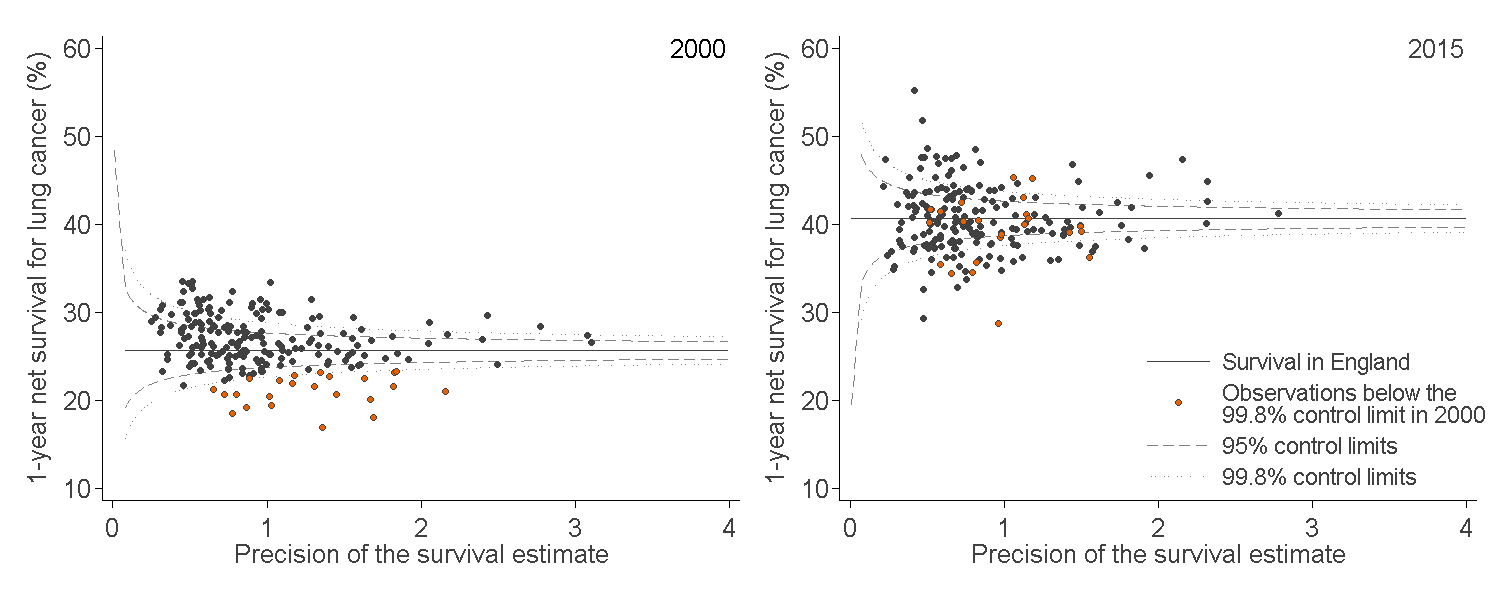
Source: National Cancer Registration and Analysis Service within Public Health England; Office for National Statistics
Notes:
Each data point represents a single CCG. The higher the precision, the more reliable the survival estimate. More information on how to interpret these funnel plots can be found in the “How to interpret a funnel plot” section.
The survival estimates identified as “outliers” fell above or below the 99.8% control limits (the wider of the two “funnels” around the England estimate) at each level of precision.
Download this image Figure 7: Funnel plot of the one-year age-sex-standardised survival (%) for lung cancer, for Clinical Commissioning Group (CCG)
.png (67.8 kB) .xls (82.9 kB)For 34 of the 207 CCGs, the one-year survival estimates were identified as being significantly lower than the England average in 2015 (Figure 8). For 29 of the CCGs, the one-year survival estimates were significantly higher than the national average. There is no obvious geographical pattern to the distribution of either group of CCGs.
Figure 8: Map of the one-year age-sex-standardised survival for lung cancer compared with the England average, for Clinical Commissioning Groups (CCG)
Adults (aged 15 to 99 years) diagnosed in 2015
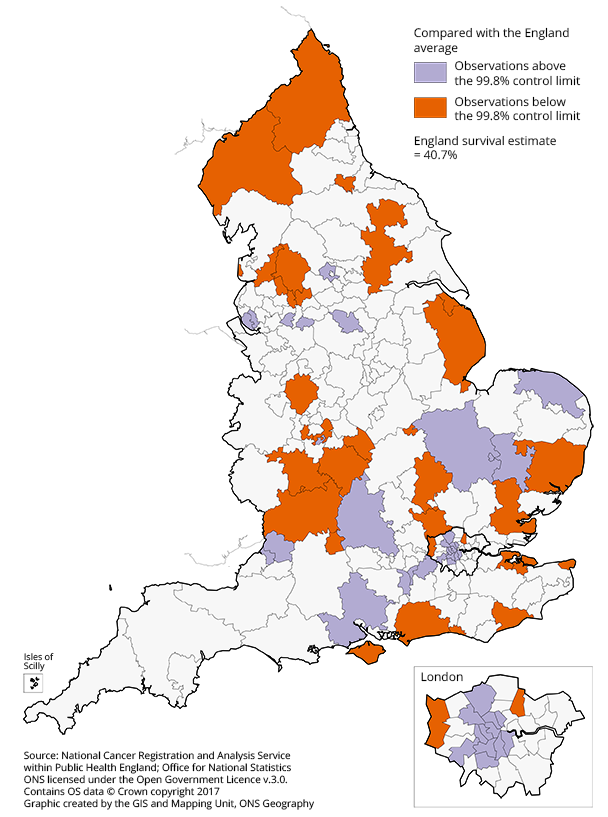
Download this image Figure 8: Map of the one-year age-sex-standardised survival for lung cancer compared with the England average, for Clinical Commissioning Groups (CCG)
.png (241.6 kB) .xls (44.5 kB)For one-year survival in STPs, the difference between the highest estimate (47.3% in Cambridgeshire and Peterborough) and the lowest estimate (36.0% in West, North and East Cumbria) for lung cancer was 11.3 percentage points.
Back to table of contents6. Interpretation of these statistics
The cancer survival index: what it is
The cancer survival index provides a convenient, single number that summarises the overall pattern of cancer survival in each Clinical Commissioning Group (CCG) or Sustainability and Transformation Partnership (STP) or England, for all cancers combined, for each calendar year. It combines the net survival estimates for each sex, age group and type of cancer (breast cancer diagnosed in women, colorectal cancer and lung cancer) separately and all other cancers combined, prostate and non-melanoma skin cancer being excluded. More information on methodology can be found in the Quality and Methodology Information report.
Research on population-based cancer survival trends in England and Wales found that for most cancers, survival is either stable or rising steadily from year to year. This trend is reflected in the index. The cancer survival index is designed to reflect real progress in cancer outcomes by long-term monitoring of progress in overall cancer survival. The index provides a summary measure of cancer survival that takes account of any shifts in the pattern of cancers in a given CCG.
The survival index can be compared over time, because it is adjusted for any changes in the profile of cancer patients by age, sex or type of cancer. This adjustment is necessary because survival varies widely by all three factors meaning that, without standardisation, changes in survival could result from changes in the profile of cancer patients. For example, overall cancer survival in a given CCG could change simply because of changes in the profile of its cancer patients, even if survival at each age, for each cancer and in each sex did not change.
Points to consider when interpreting these estimates
For geographic areas with small populations, like most CCGs, some fluctuation in survival estimates between consecutive years can be expected, as found in the following studies: Cancer survival indicators for Clinical Commissioning Groups in England and Cancer survival indicators for primary care organisations in England. Fluctuations in cancer survival by CCG can occur due to the small numbers of cancer diagnoses and deaths each year within the population. Therefore, a low survival figure for a single calendar year should not be over-interpreted. However, if the survival estimates in a given CCG are consistently low "outliers" for several years in a row, possible explanations should be considered.
Interpretation should therefore focus on trends, rather than the survival estimate for a particular year. A STP or CCG for which the survival index is consistently lower than average should nevertheless be considering why survival in its area might be low, even if it is not identified as an outlier.
The aim of this publication is to present data that can support long-term improvements in cancer control. These estimates can indicate the potential for improvement in the management of cancer, from early detection through to referral, investigation, treatment and care. Survival estimates should not be used as the only indicator of a CCG's performance in cancer outcomes. To gain a more complete picture of the cancer burden in a particular CCG, these estimates should be used alongside other information available, such as cancer incidence and mortality data.
It is important to note that CCGs in England came into existence on 1 April 2013, replacing NHS Primary Care Trusts, and STPs have been established since December 2016. A STP or CCG cannot be held responsible for trends in cancer survival that pre-date its existence. Data are provided for this 16-year period so that each CCG has a baseline against which to assess progress over time. Survival is estimated using the most up-to-date CCG boundaries – in 2016, the number of CCGs fell from 209 to 207.
CCGs are membership bodies in which local General Practitioner (GP) practices are the members. Therefore, the population of a CCG is not entirely based on the geographical population of a defined territory, but on patients who are registered with a GP practice that is a member of that CCG, but who may live in the territory of a different CCG. With this in mind, it is important to note a limitation of these analyses: the cancer patients included in the analyses are those who lived in the territory assigned to that CCG when they were diagnosed, as explained in the article, Dismantling the signposts to public health? NHS data under the Health and Social Care Act 2012.
The survival estimates must be interpreted with care. They do not reflect the survival prospects for any individual cancer patient; they represent the survival for all cancer patients in a given area, in a given period of time, diagnosed with a specified tumour.
How to interpret a funnel plot
Funnel plots offer a rapid visual presentation of variation in one-year survival estimates between CCGs, showing how they compare with one-year survival in England and taking account of the inherent variability (precision) of each survival estimate. A funnel plot avoids simply assigning a rank from 1 to 207, depending only on whether the estimate is low or high.
Small year-on-year changes in the survival estimates for a given CCG can mean big changes in its ranking. If the highest survival estimate is (say) 65% and the lowest is 50% (a 15 percentage points difference), and given that differences in the survival estimate are very small in the middle of the range, a CCG may jump 30 places up or down the ranking of 207 CCGs if the survival estimate changes by just 1% between successive years. For more information on funnel plots, please see Funnel plots for population-based cancer survival: principles, methods and applications.
Funnel plots (see Figure 9) are a useful way to identify outlying observations in cancer survival:
the black horizontal line represents the reference level or “target”, for example, the level of one-year survival in England; this is used as the reference level against which “outliers” can be identified
each data point in the plot represents the survival estimate for a given CCG (vertical scale), plotted against the precision of that estimate (the inverse of the variance) on the horizontal scale
the two “control limits”, in the shape of a funnel around the horizontal line in Figure 9, represent the expected variation in survival around the England national figure, at any given level of precision
The “outlier” observations, based on the 2000 estimates, are marked in orange (or darker; lower than expected compared with the England average).
CCGs for which the data points are within the control limits may be considered as those for which the survival estimate is no different than expected, compared with the England average and given the precision of that CCG’s estimate. Data points that fall outside the control limits are either higher or lower than expected compared with the England average.
Figure 9: An example funnel plot, one-year survival by Clinical Commissioning Group, 2015
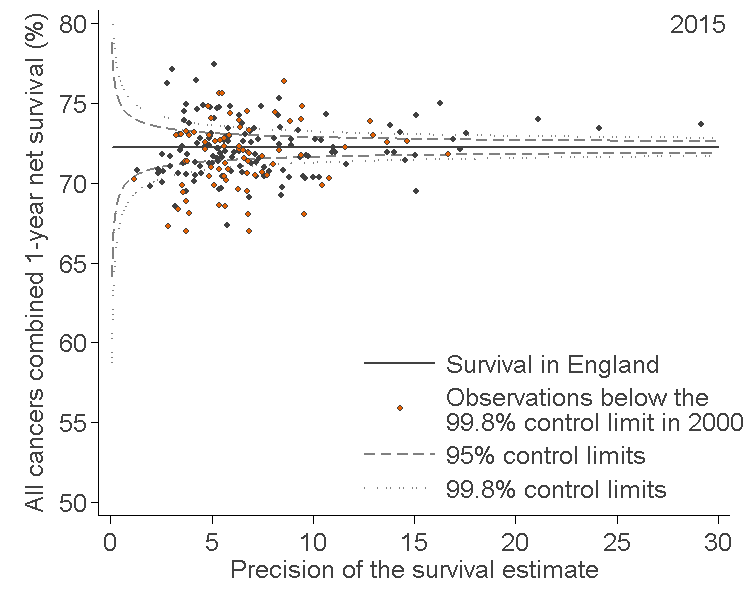
Source: National Cancer Registration and Analysis Service within Public Health England; Office for National Statistics
Notes:
Each data point represents a single CCG. The higher the precision, the more reliable the survival estimate. More information on how to interpret these funnel plots can be found in the “How to interpret a funnel plot” section.
The survival estimates identified as “outliers” fell above or below the 99.8% control limits (the wider of the two “funnels” around the England estimate) at each level of precision.
Download this image Figure 9: An example funnel plot, one-year survival by Clinical Commissioning Group, 2015
.png (43.5 kB)The precision estimate reflects the accuracy with which survival is being measured for each CCG. The higher the precision, the more reliable the estimate. Similarly, the smaller the precision, the wider the control limits, reflecting greater variability due to chance. CCGs with a large population will therefore tend to appear toward the right-hand side of each funnel plot and those with small populations on the left-hand side, closer to the vertical axis. The expected variation is shown as the 95% and 99.8% control limits (two and three standard deviations, respectively), above or below the England average.
Data points are considered an “outlier” if the value for a given CCG is lower (or higher) than would be expected by chance. If a CCG is consistently lower than the England average, then an investigation into the reasons for this may be worthwhile. This comparison is made after taking into account the age, sex and cancer profile of each CCG.
It should be noted that these “outlier” values are not just the lowest (or highest) values that would be obtained from a simple ranked list. Some of the lowest values of the index are still within the range of variation that could be expected by chance (that is, inside the control limits). These are generally for the smallest CCGs, in which the index has lower precision.
More information on the methodology can be found in the Quality and Methodology Information report.
Back to table of contents7. Who uses these statistics and for what purpose?
Given that a significant gap remains in survival compared with the European average, the Department of Health identified cancer as a specific improvement area for preventing people dying prematurely in the National Strategy (announced in 2011). In 2015, a new five-year cancer strategy for England was developed by the Independent Cancer Task Force. This sets out recommendations for how the NHS can improve cancer outcomes for patients. The implementation of these recommendations is being monitored by government bodies.
Survival estimates are used to formulate, monitor and assess health policy and healthcare provision and planning. These estimates feed into the Clinical Commissioning Group (CCG) Indicator Set, which:
“Provides clear, comparative information for CCGs, Health and Wellbeing Boards, local authorities, patients and the public about the quality of health services commissioned by CCGs and the associated health outcomes. The indicators are useful for CCGs and Health and Wellbeing Boards in identifying local priorities for quality improvement and to demonstrate progress that local health systems are making on outcomes.”
The CCG indicator set also contributes to the National Health Service (NHS) Outcomes Framework, which focuses on measuring health outcomes and includes one-year and five-year net survival from colorectal, breast and lung cancers. The NHS Five Year Forward View (2014) set out: “that improvements in outcomes will require action on three fronts: better preventions, swifter access to diagnosis, and better treatment and care for all those diagnosed with cancer.”
A detailed list of users of cancer survival estimates can be found in the Quality and Methodology Information report.
Back to table of contents9. Quality and methodology
The Index of Cancer Survival Quality and Methodology Informaton report report contains important information on:
the strengths and limitations of the data and how it compares with related data
uses and users of the data
how the output was created
the quality of the output including the accuracy of the data
All adults (aged 15 to 99 years) who were diagnosed with a first, primary, invasive malignancy were eligible for inclusion. Patients diagnosed with malignancy of the skin other than melanoma were excluded. Cancer of the prostate was also excluded from the index, because the widespread introduction of prostate-specific antigen (PSA) testing since the early 1990s has led to difficulty in the interpretation of survival trends, as explained in Excess cases of prostate cancer and estimated overdiagnosis associated with PSA testing in East Anglia.
The main change to methods since the 2016 bulletin is the adoption of new weights based on the International Classification of Survival Standard (ICSS). The benefits of incorporating the ICSS weights are:
they are publicly and readily available
these weights are widely used, for example, in the UK by Northern Ireland and Scotland and internationally by the United States National Cancer Institute and by the International Cancer Benchmark Partnership
since they are not specific to a certain country or diagnosis period, these weights could be used more widely in other countries wishing to take the same approach for an all-cancers survival index
the ICSS weights continue to vary by tumour type reflecting age distributions of the different cancers
the cancer survival in England statistical bulletin was published in June 2017 with changes in methodology, including the use of the ICSS weights; this change to the index of cancer survival for Clinical Commissioning Groups will bring consistency across ONS cancer survival estimates
To produce the all-cancers combined index, the data need to be standardised by age, sex and cancer type to allow for comparisons across the different populations. ICSS weights are used to standardise for age, with additional weighting applied to standardise for sex and cancer type.
There has been no change in the approach used for estimating survival with flexible parametric models. We are now using additional scaling tests for model selection.
The impact of these changes has been reviewed in the Impact of updating cancer survival methodologies for sub-national estimates; Index of cancer survival for Clinical Commissioning Groups in England paper.
More information on methodology can be found in the Quality and Methodology Information report.
Details of the data included in this analysis
We extracted the data used in these analyses from the cancer registration database held by NCRAS on 11 May 2017.
Patients with incomplete data (for dates of birth, diagnosis or vital status, sex, or CCG) or invalid data (non-malignant tumour behaviour or where morphology was inconsistent with the site) were excluded from analysis (3.8%). Patients were also excluded where the vital status (whether alive, emigrated, dead or not traced) on 31 December 2016 was unknown (0.3%); the cancer was only registered from a death certificate (DCO) and the survival time was therefore unknown (2.0%); or the patient had synchronous or multiple primary tumours (8.9%).
The analyses included 3,091,264 patients in total (all-cancers combined), of which 1,489,253 patients were diagnosed with breast (women), colorectal and lung cancers, constituting 48.2% of all patients included in the analyses. Patients with zero survival time (1.9% of all patients) were included in the analyses, and one day was added to their survival time.
It was sometimes impossible to produce robust estimates of survival for one or more of the age groups, most often for patients in the age group 15 to 44 years. In this situation, the missing value for a CCG is replaced by the corresponding value for their “parent” STP or, if that is also missing, the missing value for both the CCG and STP is replaced by the corresponding value for England.
For the CCG estimates, this problem affected 5,692 (17.2%) of the 33,120 separate survival estimates by age, sex, calendar year and CCG for lung cancer; 1,997 (6.0%) of the 33,120 estimates for colorectal cancer; 6 (0.0%) of the 16,560 estimates for breast cancer; and 1 (0.0%) of the 33,120 estimates for other cancers.
For the STP estimates, this problem affected 885 (5.7%) of the 15,400 separate survival estimates by age, sex, calendar year, STP and follow-up for lung cancer and 59 (0.4%) of the 15,400 estimates for colorectal cancer; it did not affect any of the estimates for breast cancer or other cancers.
CCG populations ranged from 66,854 (NHS Corby CCG) to 890,596 (NHS Northern, Eastern and Western Devon CCG), with a mean of 264,668 which can be found in the reference tables (Table 4 for all-cancers combined).
Further information regarding the applied methodology is available in the following publications:
Corazziari I, Quinn M, Capocaccia R (2004) ‘Standard cancer patient population for age standardising survival ratios’, European Journal of Cancer, Volume 40, pages 2,307 to 2,316
Lambert PC, Royston P (2009), ‘Further development of flexible parametric models for survival analysis’, Stata Journal, Volume 9, pages 265 to 290
Li, R and others (2014), ‘Control of data quality for population-base cancer survival analysis’, Cancer Epidemiology, Volume 38, pages 314 to 320
Martos C and others (2014), ‘A proposal on cancer data quality checks: one common procedure for European cancer registries’, European Commission, Joint Research Centre
Royston P, Parmar MK (2002), ‘Flexible parametric proportional-hazards and proportional-odds models for censored survival data, with application to prognostic modelling and estimation of treatment effects’, Stat Med, Volume 21, Issue 15, pages 2,175 to 2,197
Quaresma M, Coleman MP, Rachet B (2014), ‘Funnel plots for population-based cancer survival: principles, methods and applications’, Stat Med, Volume 33, pages 1,070 to 1,080
11. Acknowledgements
This work uses data provided by patients and collected by the NHS as part of their care and support. All personal data is handled confidentially by ONS and PHE, in accordance with relevant legislation and codes of conduct.
Back to table of contents
