1. Main points
Public service adult social care productivity fell by 0.6% in financial year ending (FYE) 2018, as inputs rose by 0.4% and output fell by 0.2%
Inputs growth slowed from 0.7% in FYE 2017 to 0.4% in FYE 2018 due to an increase in input inflation, largely driven by faster labour cost growth
Output fell by 0.2% in FYE 2018 due to falls in both the quantity and quality of output of 0.1%. This was the first fall in the quality adjustment since its introduction in FYE 2011
Residential and nursing care, which accounts for nearly one-third of public adult social care expenditure, experienced a 1.8% fall in productivity in FYE 2018 as output fell by more than inputs
Residential and nursing care output fell in every measured year between FYE 2005 and FYE 2018 while output provided through direct payments rose in every measured year since they were first included in FYE 2001
Overall public service adult social care productivity was 8.4% lower in FYE 2018 than FYE 1997, although most of this fall occurred during the decade of the 2000s
The productivity of working age adults’ care fell by more than older adults’ care over the whole series, although since FYE 2010 the productivity of working age adults’ care has performed better, partly due to better quality improvements for this age group
2. Things you need to know about this release
Public service productivity is estimated by comparing growth in the total quantity of inputs used with growth in the total quantity of output provided, adjusted for the quality of this output. If the growth rate of output exceeds the growth rate of inputs, productivity increases, meaning that more output is being produced for each unit of input. Conversely, if the growth rate of inputs exceeds the growth rate of output, then public service productivity will fall, indicating that less output is being produced for each unit of input.
Inputs are composed of labour, goods and services, and capital consumption, and are measured on a volume basis using expenditure adjusted for the specific cost inflation rates faced by adult social care (ASC) inputs.
Quantity output is measured as the number of individual activities performed weighted by their cost, where activity data are available, and where activity data are not available, output is measured using the equivalent deflated expenditure data as inputs. A quality adjustment is applied to output to account for changes in service quality.
Whilst these productivity estimates provide a measure of the amount of output that is produced for each unit of input, they do not measure value for money, whether inputs have been obtained for the lowest possible cost, or whether most appropriate forms of care have been used.
This publication focusses on adult social care (ASC). ASC services provide care and support to older people, adults with learning or physical disabilities, adults with mental health problems, drug and alcohol misusers, and carers. ASC services include:
- placements in residential and nursing care
- provision of home care services
- day care services
- supported living and accommodation
- “meals on wheels"
- equipment and home adaptions
- care assessments and support services
The term “public service” is used as this publication only covers publicly funded ASC services. Privately funded ASC services are excluded from input, outputs and productivity. However, publicly-funded services provided by independent sector providers are included.
There have been several changes in the data sources over time:
- data on funding for social care received by local authorities from the NHS was not available prior to financial year ending (FYE) 2005; local authority-provided or -arranged social care activity funded by the NHS is only incorporated in the growth of inputs and output from FYE 2005 onwards
- the source for the quality adjustment, the Adult Social Care Survey, was introduced in FYE 2011, and so the quality adjustment is first applied to output growth between the years FYE 2011 and FYE 2012
- there was a change in how social care data was collected between FYE 2014 and FYE 2015 which affected financial, activity and quality data; as a result, changes in productivity and the quality adjustment cannot be measured and output is assumed to grow at the same rate as inputs between these two years
- from FYE 2014 onwards, activity data are not available for referrals and assessments and community care services, such as home care and day care, and so output is assumed to be equal to inputs and productivity changes cannot be estimated after FYE 2014 for these services
- due to a change in the unit of activity used to record short-term care to maximise independence between FYE 2017 and FYE 2018, changes in the productivity of short-term care cannot be measured and short-term care output is assumed to grow at the same rate as inputs between these two years
Due to the use of chain-linking to produce input and output indices, these changes do not result in a jump in the level of input and output indices. Instead, these changes are incorporated in the growth rate of the relevant indices, enabling the levels of output, inputs and productivity to be analysed across the series.
While much of the data used in the measure are also used in the production of the national accounts, methodological changes mean that both output and inputs in this publication are inconsistent with the national accounts. Recent data source and relevant methods changes made to produce this article will be incorporated into the national accounts at a point in the future. Further information about the data and methods used to produce these estimates can be found in Public service productivity: adult social care, current method, 2019 update and in Public service productivity: adult social care: Quality and methodology information.
Back to table of contents3. Productivity
Figure 1 shows changes in the growth rate and trend of public service adult social care productivity over time, while Figure 2 shows how the productivity growth rate has been driven by changes in inputs and output.
In these charts, annual growth rates are shown as bars and measured against the right axis. Cumulative changes in each series since financial year ending (FYE) 1997 are shown by the lines, measured against the left axis and indexed to a level of 100 in FYE 1997.
Figure 1: Public service adult social care productivity, FYE 1997 to FYE 2018
England
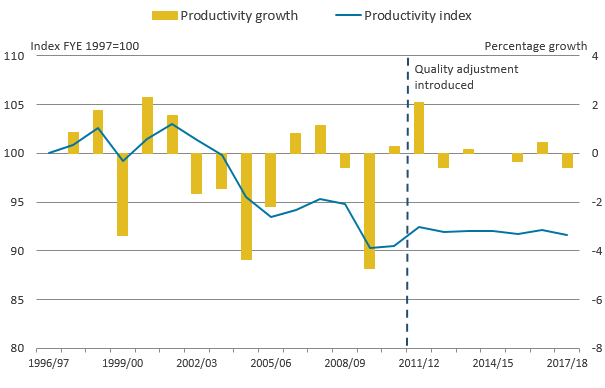
Source: Office for National Statistics
Notes:
- Quality adjustment applies after financial year ending 2011.
- For FYE 2015, productivity is not estimated due to a break in series.
Download this image Figure 1: Public service adult social care productivity, FYE 1997 to FYE 2018
.png (17.1 kB) .xls (26.6 kB)
Figure 2: Public service adult social care inputs and output, FYE 1997 to FYE 2018
England
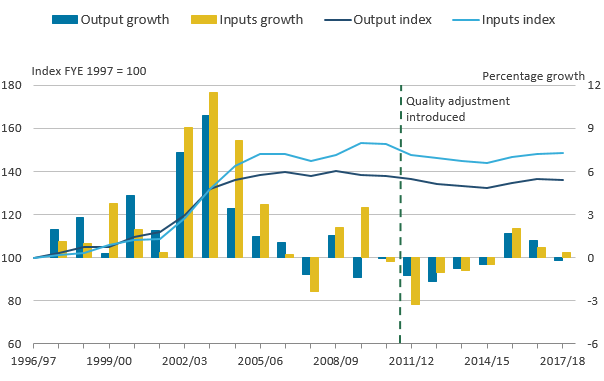
Source: Office for National Statistics
Notes:
- There is a break in series between FYE 2011 and FYE 2012 indicated by the dotted green line, and accompanying text "quality adjustment introduced".
Download this image Figure 2: Public service adult social care inputs and output, FYE 1997 to FYE 2018
.png (15.7 kB) .xls (38.9 kB)Figure 1 shows that productivity across public service adult social care (ASC) fell by 0.6% in FYE 20181 , reversing the productivity growth of 0.5% seen in FYE 2017. This fall was caused by the combination of a small fall in output of 0.2% and a small increase in inputs of 0.4%.
Figure 1 shows that overall, ASC productivity is 8.4% lower in FYE 2018 than it was in FYE 1997. This means that 8.4% less output was provided for each unit of input in FYE 2018 than it was in FYE 1997.
Lower productivity at the end of the series than its start can largely be traced to the period between FYE 2002 and FYE 2006, when there was a large increase in output but an even larger increase in input, resulting in a fall in productivity.
It should be noted that due to a change in the data source between FYE 2014 and FYE 2015, productivity change cannot be measured between these two years. Furthermore, following this change from FYE 2015 onwards, it is not possible to measure output and productivity growth using our preferred “directly measured” methodology for most community care services, such as home care and day care. As a result, we produce a separate productivity measure for directly measured services only, which, in FYE 2018, consists of residential and nursing care. Productivity for directly measured services fell by 1.8% in FYE 2018. More information on these directly-measured productivity estimates can be found in Section 8, while separate productivity estimates, also produced on a directly measured basis for different client groups and service types are in Section 9 and Section 10.
Figure 2 shows that the quantity of both inputs used and output provided have changed little since FYE 2006. This is despite an increase between 2006 and 2017 in the population of England of 9.6% and a 24.0% increase in the population aged over 65 years, an age group who are more likely to require social care. The relatively constant level of output since FYE 2006 is in contrast to the number of care clients, which has fallen substantially over the period. The reason output has not fallen similarly is likely to be a shift in the balance of care provision from lower-need to higher-need clients2.
It should be noted that this publication covers only publicly funded3 and not privately funded ASC activity, and so cannot measure the total amount of ASC services consumed.
Notes for: Productivity
Growth rates for a single year are given as the growth between the stated year and previous year. For example, the growth figure for FYE 2018 is the growth measured between FYE 2017 and FYE 2018. Growth rates for a period of more than one year are given as the growth between the first and the last year in that period. For example, growth between FYE 2016 and FYE 2018 represents growth between the level of a series in FYE 2016 and its level in FYE 2018.
More information on changes in the intensity of care is available from research by the Centre for Analysis of Social Exclusion (CASE) at the London School of Economics (LSE).
The measure includes local authority-provided or -arranged care funded by local authorities or by payments from the NHS. It does not include other NHS services for people with long-term conditions which are organised without local authority involvement.
4. Inputs
Figure 3 shows changes in the inputs used in providing publicly funded adult social care (ASC). These inputs cover the labour, intermediate consumption of goods and services, and capital used by local authorities in providing ASC services and care purchased by local authorities from independent sector providers. Analysis of the inputs data is useful to understand the resources available to provide ASC services.
Figure 3: Public service adult social care inputs, FYE 1997 to FYE 2018
England
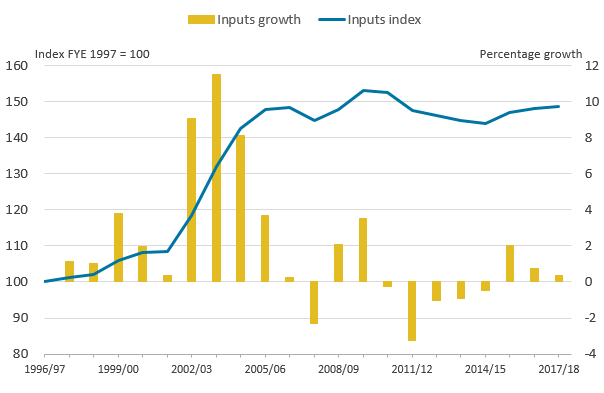
Source: Office for National Statistics
Download this image Figure 3: Public service adult social care inputs, FYE 1997 to FYE 2018
.png (16.8 kB) .xls (27.1 kB)Figure 3 shows that inputs grew by 0.4% in financial year ending (FYE) 2018. This was the third consecutive year of inputs growth since FYE 2015, following a period between FYE 2010 and FYE 2015, which recorded five consecutive years of falling inputs.
While the level of inputs in FYE 2018 is nearly 50% higher than in FYE 1997, most of this increase occurred between FYE 2002 and FYE 2006. The level of inputs in FYE 2018 was only 0.4% higher than in FYE 2006.
While expenditure on ASC services has nearly trebled in current price terms since FYE 1997, input costs have nearly doubled, leaving ASC inputs only about 50% higher than in FYE 1997
The quantity of inputs is calculated by adjusting ASC expenditure by the specific inflation rate that applies to that element of inputs, a process known as deflation. Figure 4 shows how changes in expenditure and inflation have affected inputs growth.
Figure 4: Input expenditure and inflation for public service adult social care inputs, FYE 1997 to FYE 2018
England
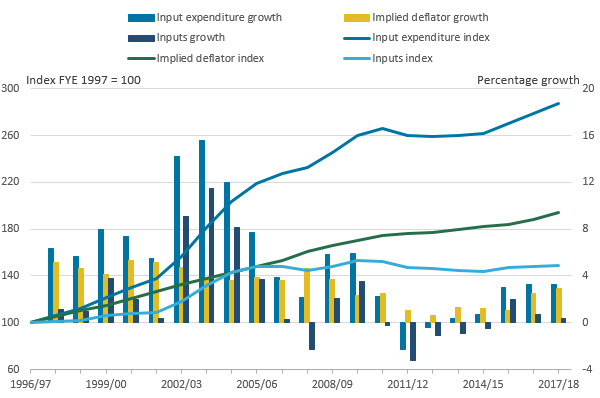
Source: Office for National Statistics
Notes:
- There is a break in series between FYE 2004 and FYE 2005 due to NHS funding being included in the expenditure growth from FYE 2005 onwards. Due to the use of chain-linking, these changes affect the growth rate of expenditure but do not result in a jump in the level of expenditure.
Download this image Figure 4: Input expenditure and inflation for public service adult social care inputs, FYE 1997 to FYE 2018
.png (25.9 kB) .xls (38.4 kB)Figure 4 shows that, in current price terms, public expenditure on ASC services was 188% or nearly three times higher in FYE 2018 than in FYE 1997. However, over the same period, the cost of ASC inputs increased by 94%, meaning the price level for ASC inputs nearly doubled. As a result, the quantity of inputs used in providing ASC rose by just under 50%.
Most of the increase in current price expenditure over the series occurred between FYE 1997 and FYE 2010. Current price expenditure experienced little change between FYE 2010 and FYE 2015. However, inflation in input costs was also at its lowest level over the series during this period, which limited the fall in ASC inputs.
Faster current price expenditure growth resumed in FYE 2016. This is likely to be partly due to the introduction of the Better Care Fund in FYE 2016. The Better Care Fund is a transfer from the NHS to local authorities which aims to improve efficiency and outcomes across health and social care by facilitating closer co-ordination between the two services.
While current price expenditure on ASC services increased at 3% or more per year each year since FYE 2016, the effect of this faster expenditure growth on inputs diminished in FYE 2017 and FYE 2018 as a result of faster input cost inflation. Input cost inflation reached 2.9% in FYE 2018, its highest rate since FYE 2009.
Local authorities’ purchases of care from other providers has increased from half of spending to three-quarters of spending between FYE 1997 and FYE 2018
Publicly funded ASC services covered in this article can be provided by local authorities or independent sector providers. Figure 5 shows how public expenditure on ASC services is split between local authorities’ own provision and care provided by others. Care provided by others mainly consists of care commissioned from independent sector providers1 .
Figure 5: Analysis of public expenditure on adult social care by provider type, FYE 1997 to FYE 2018
England
Source: Office for National Statistics
Notes:
- There is a break in series between FYE 2014 and FYE 2015 due to a change in data collection.
Download this chart Figure 5: Analysis of public expenditure on adult social care by provider type, FYE 1997 to FYE 2018
Image .csv .xlsFigure 5 shows that the proportion of spending accounted for by local authority own provision, as opposed to care provided by others, decreased from just over half of publicly funded ASC in FYE 1997 to one-quarter in FYE 2018.
In FYE 2018, labour cost inflation reached its highest rate in 10 years for independent sector providers, as the National Living Wage rose
Figure 6 shows the main deflators applied to the expenditure data to calculate ASC inputs. The height of the indices represents how much higher the price level for each deflator is relative to its level in FYE 1997. Faster growth in a deflator series means fewer inputs can be purchased for each pound of spending, and so higher deflator growth results in lower input growth for any given rate of spending growth.
Figure 6: Deflators used in adult social care inputs, FYE 1997 to FYE 2018
England
Source: Office for National Statistics, Department for Health and Social Care, Skills for Care, LaingBuisson, UK Home Care Association, Ministry for Housing, Communities and Local Government
Download this chart Figure 6: Deflators used in adult social care inputs, FYE 1997 to FYE 2018
Image .csv .xlsFigure 6 shows that over the period since FYE 1997, labour costs have increased more than the cost of the intermediate consumption of goods and services.
Labour costs account for the majority of ASC inputs, with independent sector labour costs accounting for the largest input share of any of the deflators for most of the period. As a result of a change2 in the data source for the labour deflators from the Annual Survey of Hours and Earnings to the National Minimum Dataset for Social Care in FYE 2014, it is possible to estimate fully separate labour deflators for the local authority and independent sector from this date. It should be noted that differences between the two series before FYE 2014 are only due to differences in the mix of staff groups employed in each sector and so do not show the full difference between local authority and independent sector cost inflation.
Figure 6 shows that the labour costs of independent sector providers grew considerably faster than local authority labour costs from FYE 2015 onwards. This may be due to relatively large increases in the National Living Wage and National Minimum Wage since October 2014.
As independent sector providers are more likely to employ staff at the minimum wage, increases in the minimum wage have a greater effect on independent sector labour costs. Data from Skills for Care show that in March 2016, 39% of care workers in the independent sector were paid less than £7.20 an hour, the rate that the National Living Wage rose to in April 2016, and a similar effect was found in April 2017. In contrast, only 1% of local authority care workers were paid below this rate and so the effect of changes in the National Living Wage are smaller on local authority care workers.
However, it should also be noted that it is also possible that this divergence may be partly related to a change in the data source for pay growth from FYE 2014 onwards from the Annual Survey of Hours and Earnings to the National Minimum Data Set for Social Care, which is a specific data collection from care providers.
Increasing labour input costs are not the only driver of increasing input inflation. Deflators for intermediate consumption of goods and services are produced using data from a range of sources, including the Office for National Statistics, LaingBuisson, the UK Home Care Association and the Ministry of Housing, Communities and Local Government. The increasing inflation in the most recent years observed in Figure 4 is also partly due to stronger inflation in the intermediate consumption of goods and services, particularly the costs of transport, food and insurance.
More information on the deflators used in the inputs can be found in Public service productivity: adult social care, current method, 2019 update, while further breakdowns of these deflators are available in the Reference Tables.
In FYE 2018, ASC input inflation increased to a rate 0.9 percentage points faster than inflation in the general economy
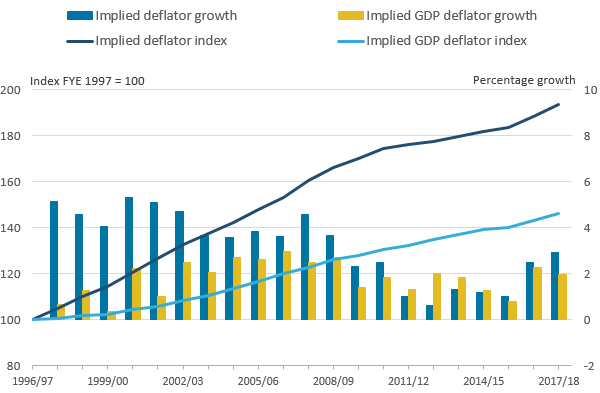
Figure 7 compares the inflation rate experienced by adult social care inputs relative to the inflation rate of the general economy, measured by the implied gross domestic product (GDP) deflator.
Figure 7: Implied deflators for adult social care inputs and the overall economy, FYE 1997 to FYE 2018
England
Source: Office for National Statistics
Download this image Figure 7: Implied deflators for adult social care inputs and the overall economy, FYE 1997 to FYE 2018
.png (25.2 kB) .xls (28.7 kB)Figure 7 shows that between FYE 1997 and FYE 2018, the total inflation experienced by adult social care inputs was approximately double that for the general economy. Much of this divergence occurred between FYE 1997 and FYE 2010, largely due to rising real wages of adult social care workers. Between FYE 2011 and FYE 2014, the real wages of the ASC workforce, along with real wages across the whole economy, fell. As labour costs make up most ASC inputs, falling real wages in ASC meant inflation in ASC inputs was lower than that of the general economy over this period.
However, ASC input inflation has been greater than inflation in the general economy over the last three years. In FYE 2018, ASC input inflation was 0.9% higher than inflation in the general economy, the greatest amount by which ASC input inflation has exceeded the implied GDP deflator since FYE 2010.
Notes for: Inputs
In addition to care provided by independent sector providers, care provided by others also includes care commissioned by local authorities from other local authorities, although this is understood to consist of only a small part of the care provided by others category.
As with other breaks in series used in the productivity measure, the use of chain-linking means this change does not result in a step-change in the deflators.
5. Output quantity
Figure 8 shows the quantity of public service adult social care (ASC) output provided.
For services where activity data are available, the quantity of ASC output is measured by calculating the growth rates of different adult social care (ASC) activities and weighting these by their unit costs. As a result, growth in activities that are high-volume and expensive has a greater effect on the output index than a similar rate of growth in activities that are uncommon and low-cost.
To produce output, ASC activities are differentiated by the type of service, such as weeks in residential care or hours of home care. Residential, nursing and day care, and referrals and assessments are further differentiated by client age group and reason for needing care as differing care needs result in different costs of care provision.
For service types where activity data are not available, output growth is assumed to be equal to inputs growth.
Data in Figure 8 is non-quality adjusted and the quality adjustment is introduced in Section 6.
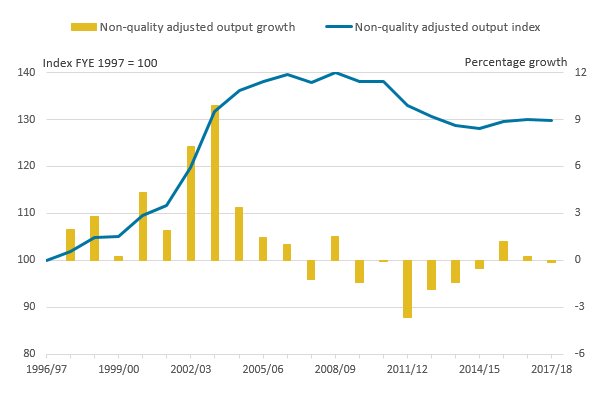
Figure 8: Public service adult social care non-quality adjusted output, FYE 1997 to FYE 2018
England
Source: Office for National Statistics
Download this image Figure 8: Public service adult social care non-quality adjusted output, FYE 1997 to FYE 2018
.png (15.4 kB) .xls (26.6 kB)Figure 8 shows that the quantity of publicly funded ASC services provided was 30% higher in FYE 2018 than in financial year ending (FYE) 1997. However, the increase in ASC quantity output was not continuous over this period and can be divided into several distinct phases:
- quantity output increased by every year between FYE 1997 and FYE 2007, increasing by 40% in total over this period
- quantity output then changed little between FYE 2007 and FYE 2011
- between FYE 2011 and FYE 2015, quantity output fell by 7.2%
- quantity output grew again in FYE 2016, the year the Better Care Fund was introduced and inputs also rose, and quantity output remained relatively unchanged in FYE 2017 and FYE 2018
As mentioned in Section 3, changes in ASC output can be seen in the context of changes in the population requiring care.
Between mid-1996 and mid-2017, the population of England increased by 14.6%, while the population aged over 65 years increased by 30%. Looking at the period from FYE 2007 to FYE 2018, over which the quantity of ASC services provided fell by 7.0%, the whole population of England increased by 9.6% and the population aged over 65 years increased by 24%1 .
It should be noted that changes in the whole population or the population over a certain age provide little precision in quantifying changes in population care needs. Care needs generally increase with age, with people aged 85 years more likely to require ASC assistance than people aged 65 years2 .
In addition, more than half of public expenditure on ASC is on working age adults (defined as those aged between 18 and 64 years), with most ASC expenditure on working age adults supporting adults with learning disabilities. Figures from Public Health England on patients registered with their GP as having a learning disability have risen in recent years from 139,000 in FYE 2007 to 214,000 in FYE 2014. This indicates an increase in care needs for the working age group beyond population growth, although this rise may be partly due to improvements in GP recording. Emerson and Hatton (2011) project changes in the provision of ASC services for adults with learning disabilities will have to grow by between 1.2% and 5.1% in the 18 years up to 2030, above the rate of general population growth.
As the public service ASC productivity measure covers only publicly funded care, output will also be affected by the wealth of people in need of care, due to the use of personal wealth thresholds in determining how much of care costs are paid by local authorities.
The inclusion of only publicly funded care in the measure also means that it excludes privately funded care and unpaid care provided by family members, friends and volunteers. Both privately funded and unpaid care are considerably more difficult to obtain comprehensive data on than publicly-funded care.
The UK health accounts provide data on long-term care spending, which covers most ASC expenditure, although also includes additional elements of hospital and other spending. These data show that private3 and charitable expenditure on long-term care increased by 15.4% between 2013 and 2016, relative to public expenditure (excluding Carer’s Allowance) which increased by 9.2%.
Data from the Household Satellite Accounts suggest the total number of informal care hours received by adults rose from 6.4 billion in 2005 to 8.5 billion in 2013, before falling back to 7.9 billion in 2016. It should be noted that these figures mainly include continuous care and only a small proportion of the total hours received relate to personal and practical care that many ASC home care services provide.
Therefore, while these figures suggest that an increase in private and charitable expenditure may be meeting some of the growing need for care, there is little apparent growth in unpaid care and we cannot confirm that private, charitable and unpaid sources account for the apparent fall in publicly funded output relative to growing care needs.
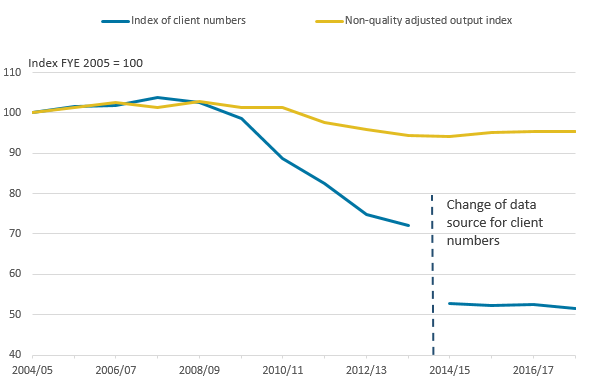
Figure 9: Public service adult social care non-quality adjusted output and client numbers, FYE 2005 to FYE 2018
England
Source: Office for National Statistics
Notes:
- There is a break in series in the number of clients receiving long-term support at year-end between FYE 2014 and FYE 2015 due to a change in data source. Prior to FYE 2014, this measure is the sum of clients in receipt of community or residential or nursing care at year-end. Between FYE 2015 and FYE 2018, the index of client numbers shows the numbers receiving long-term support at the year-end.
- The Index of clients receiving long-term support services at year-end is indexed to the number of clients in receipt of community or residential or nursing care in FYE 2005, although levels before and after the break in series are not comparable.
Download this image Figure 9: Public service adult social care non-quality adjusted output and client numbers, FYE 2005 to FYE 2018
.png (13.6 kB) .xls (27.6 kB)Figure 9 shows that while the quantity of output has declined, the number of clients receiving care has declined more. This is likely to be due to the fall in client numbers being attributable to clients with lower-intensity needs as shown by research by the Centre for Analysis of Social Exclusion (CASE) at the London School of Economics (LSE). As the output measure is a combination of cost-weighted activity and deflated expenditure, a reduction in low-intensity care, such as relatively low-frequency home care visits, will have less of an effect on output than on client numbers.
Residential and nursing care output has declined since FYE 2006, while care provided through direct payments has increased in every recorded year since these were first measured in FYE 2001
Figure 10 shows how different service types have driven changes in public service ASC output over the series. More information on how output growth is calculated can be found in Section 2 and Public service productivity: adult social care, current method, 2019 update and information on productivity and the proportion of expenditure by service type can be found in Section 10.
It should be noted that due to a change in data collections between FYE 2014 and FYE 2015, it is not possible to analyse the contributions of individual service types to ASC output growth between these two years, with total output growth measured on the “output-equals-inputs” basis.
Figure 10: Contributions to public service adult social care output growth, FYE 1997 to FYE 2018
England
Source: Office for National Statistics
Notes:
- In the ASC output measure, residential care, nursing care, community care – home care, community care – day care, community care – other directly measured and referrals and assessments are measured directly, and direct payments and other indirectly measured services are measured indirectly.
- Expenditure on direct payments was first separately recorded in the data in FYE 2001.
- There is a break in series between FYE 2014 and FYE 2015 due to a change of data collection, resulting in most community services being measured indirectly from FYE 2015 on.
- Due to the break in series between FYE 2014 and FYE 2015, output growth is indirectly measured for all services for FYE 2015, and therefore it is not possible to calculate contributions to growth for individual service types for this financial year.
- Up until FYE 2014, other directly measured provision included meals, as well as equipment and adaptations. From FYE 2015, this category includes only short-term care to maximise independence.
- Due to a change in how activity data was recorded for short term care to maximise independence in FYE 2018, this category of provision is indirectly measured for FYE 2018, and is included in the other indirectly measured category in FYE 2018.
- The sum of components of output will might not add up to the total output due to rounding.
Download this chart Figure 10: Contributions to public service adult social care output growth, FYE 1997 to FYE 2018
Image .csv .xlsFigure 10 shows how residential and nursing care made a positive contribution to output growth for most of the period between FYE 1997 and FYE 2005. However, since FYE 2006, the combined effect of residential and nursing care on output has been negative in every year measured.
In contrast, direct payments have increased output growth in each year of the series they have been recorded. Direct payments involve local authorities providing funding to care clients to enable them to arrange and pay for the care themselves, in place of the local authority commissioning the care for them4. This often enables clients to receive a more personalised service tailored to their needs.
Except for FYE 2015, where there is a break in series, direct payments contributed at least 0.5% per year to total output growth over the period between FYE 2004 and FYE 2016. The contribution to total output growth from direct payments was lower in the last two years of the series due to slower growth in direct payment output but was still positive.
The change in data collection after FYE 2014, means that it is no longer possible to directly measure output for referrals and assessments or for community care services such as day care and home care, and so these are only measured indirectly after FYE 2014. For the period available, the data show that output for home care, day care and other directly measured community services all made a negative contribution to overall output growth in every year between FYE 2011 and FYE 2014.
Other indirectly measured services covers ASC services for which no activity data are available, such as supported accommodation until FYE 2014 and supported accommodation, home care, day care and other long-term community services, and commissioning and service delivery after FYE 2014. Other indirectly measured services made positive and negative contributions to overall output growth at different points in the series, but have made positive contributions to output growth in each of the last three years of the series.
Notes for: Output quantity
- Population figures are mid-year estimates for 2006 and 2017.
- More information on how care needs change with age is available from the English Longitudinal Study on Ageing
- Private expenditure includes client contributions to the cost of local authority-provided or -arranged ASC services, which are excluded from the public service ASC productivity measure.
- More information on direct payments is available from the House of Commons Library
6. Output quality
Figure 11 shows how applying a quality adjustment changes public service adult social care (ASC) output growth.
The quality adjustment is based on the concept of adjusted social care-related quality of life and produced using data from the Adult Social Care Survey (ASCS). This quality adjustment measures changes in how well care clients’ needs are met across domains of quality of life affected by social care, while controlling for factors outside the control of ASC services which may also affect quality of life. This enables the estimation of changes in care clients’ quality of life which are due to changes in the quality of local authority-provided or -arranged ASC services.
Due to data availability, the change in quality is first calculated for FYE 2012. Due to a change to the ASCS between FYE 2014 and FYE 2015, no quality change can be calculated for FYE 2015.
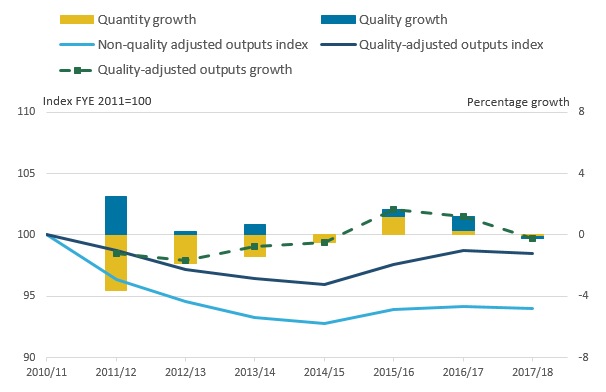
Figure 11: Output quality adjustment, FYE 2011 to FYE 2018
England
Source: Office for National Statistics
Notes:
- Quality growth is not estimated for FYE 2015 due to a break in series.
Download this image Figure 11: Output quality adjustment, FYE 2011 to FYE 2018
.png (18.4 kB) .xls (34.8 kB)Figure 11 shows that the quality adjustment fell by 0.1% in FYE 2018, having made a positive contribution to output and productivity growth in each of the previous years it was available.
Table 1 shows the change in the quality adjustment broken down by service type and client group.
| Percentage growth | |||||||
|---|---|---|---|---|---|---|---|
| FYE 2012 | FYE 2013 | FYE 2014 | FYE 2015 | FYE 2016 | FYE 2017 | FYE 2018 | |
| Overall quality adjustment | 2.5 | 0.2 | 0.7 | 0.0 | 0.5 | 0.9 | -0.1 |
| Residential and nursing care - all adults | 0.7 | 0.1 | -0.6 | 0.0 | 0.6 | 0.3 | -0.4 |
| Community care - all adults | 3.9 | 0.3 | 1.7 | 0.0 | 0.4 | 1.4 | 0.1 |
| All social care - older adults | 1.8 | 0.8 | 0.0 | 0.0 | 0.0 | 1.1 | 0.0 |
| All social care - working age adults | 3.1 | -0.3 | 1.3 | 0.0 | 0.9 | 0.8 | -0.2 |
Download this table Table 1: Growth in components of adult social care quality adjustment, FYE 2012 to FYE 2018
.xls .csvThe fall in quality in FYE 2018 was caused by a fall in the quality adjustment of residential and nursing care of 0.4%, while the quality adjustment for community care grew by only 0.1%, its slowest growth over the series.
Overall the quality adjustment reduced the fall in output between FYE 2011 and FYE 2018 from 6.0% to 1.5%. This positive quality adjustment indicates an increase in social care-related quality of life attributable to improved ASC service quality.
Back to table of contents7. Quality and non-quality adjusted ASC productivity
Figure 12 brings together adult social care (ASC) inputs and output quantity and quality to produce productivity.
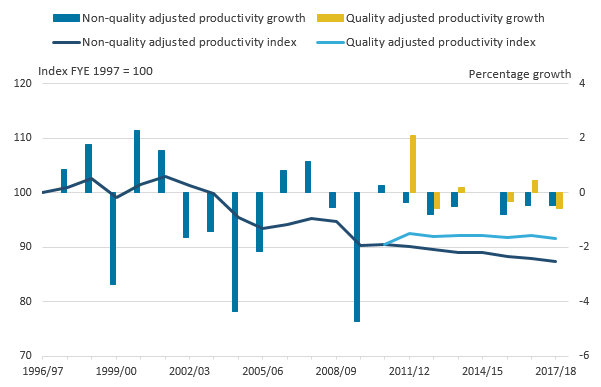
Figure 12: Public service adult social care productivity, quality and non-quality adjusted, FYE 1997 to FYE 2018
England
Source: Office for National Statistics
Download this image Figure 12: Public service adult social care productivity, quality and non-quality adjusted, FYE 1997 to FYE 2018
.png (18.2 kB) .xls (28.2 kB)Figure 12 shows that between financial year ending (FYE) 1997 and FYE 2011, ASC productivity, which was without quality adjustment for these years fell by 9.5%. After the introduction of the quality adjustment, quality adjusted productivity grew by 1.2% between FYE 2011 and FYE 2018 and non-quality adjusted productivity fell by 3.4%.
The fall in ASC productivity between FYE 1997 and FYE 2011 could be due to a deterioration in the efficiency of service provision. However, there are other possible factors which could influence the fall in the productivity measure.
The ASC productivity estimates aim to capture the effect of care clients with more intense needs requiring more expensive care within the output measure. This is done by separately measuring the output of residential, nursing and day care, and referrals and assessments by client age group and the reason they require support1 . However, there will be variation in the intensity of care for clients within each client age group and support reason, which will not be captured within the productivity measure.
The National Audit Office points to demographic factors, such as ageing, being responsible for increasing the number of clients with high-intensity needs. If clients with high-intensity needs are making up a greater proportion of care clients within each client support need group, the output measure may understate growth and the productivity measure may overstate the fall in productivity.
In addition, the data used for the quality adjustment are not available for the period before FYE 2011, the period during which productivity fell. Figure 12 shows that quality adjusted productivity does not fall over the period for which we have data, unlike non-quality adjusted productivity, which continues to fall, albeit at a slower rate than during the previous decade. It is possible that had an ASC output quality adjustment been available for earlier years, this would have limited the fall in productivity.
Section 8 discusses a further reason for the slower falls in productivity experienced from FYE 2015 onwards, which relates to the methodology used for output.
Notes for: Quality and non-quality adjusted ASC productivity
- For home care, separate client groups do not need to be used, as hours of care provided is used within the output and this unit of activity reflects the intensity of care needed.
8. Productivity of directly measured ASC services
As discussed in Section 5, where activity data are available, these are weighted by their costs to produce output. This is known as directly measured output. Where activity data are not available, output growth is estimated to equal input growth, and this is known as indirectly measured output.
Directly measured output is preferred as it enables the calculation of productivity change. However, by estimating output to be equal to inputs, no productivity change can be observed for indirectly measured output.
While using both directly and indirectly measured output is necessary to ensure total output growth can be measured, the inclusion of indirectly measured output also reduces the scale of changes in the overall productivity measure. Therefore, where productivity is falling for both directly and indirectly measured services, but this fall can only be measured for directly measured services, the use of indirectly measured output results in an underestimation of the fall in productivity.
Following a data source change between financial year ending (FYE) 2014 and FYE 2015, the proportion of adult social care (ASC) services for which directly measured output can be used was smaller. This is shown by Figure 13.
Figure 13: Proportion of public expenditure on ASC services for which activity data are available, FYE 1997 to FYE 2018
England
Source: Office for National Statistics
Notes:
- The change in data collection prevents any directly measured output to be calculated for FYE 2015. Figures are given as the proportion of output which is directly measured for the purpose of calculating output growth between the stated year and the previous year. Because output is produced using a Laspeyres index, growth between two years is weighted using data from the first year of each two-year pair. Therefore, as an example, the figure for FYE 2017 refers to the proportion of output that is directly measured for the purpose of calculating output growth between FYE 2016 and FYE 2017, which is calculated from FYE 2016 expenditure data.
- The proportion that is directly measured falls in FYE 2018 as a result of a change in the reporting of short-term care activity, which means that short-term care to maximise independence output cannot be directly measured for FYE 2018.
Download this chart Figure 13: Proportion of public expenditure on ASC services for which activity data are available, FYE 1997 to FYE 2018
Image .csv .xlsFor output growth in FYE 2014, activity data were available for about three-quarters of public expenditure on ASC services, whereas in FYE 2016, activity data was available for only around one-third of expenditure. This means that, following the data source change, productivity growth cannot be measured for a larger share of ASC services after FYE 2015, and hence the underestimation of falls in ASC productivity may be greater after this point.
By changing the input and output measures such that both only cover services for which activity data are available, it is possible to produce a productivity measure where the scale of productivity changes are not reduced by the inclusion of indirectly-measured output. The downside to this approach is that input and output series no longer cover all ASC services.
Figure 14 shows the ASC productivity measure for directly measured services only in comparison to the overall ASC productivity measure.
Excluding services for which productivity cannot be measured, non-quality adjusted ASC productivity fell by 5.0% between FYE 2015 and FYE 2018, compared with 1.8% for the overall non-quality adjusted productivity measure
Figure 14: Quality and non-quality adjusted productivity for directly-measured ASC services only and all ASC services, FYE 1997 to FYE 2018
England
Source: Office for National Statistics
Notes:
- Directly measured activity includes: residential and nursing care throughout the series, with the exception of FYE 2015; home care, referrals and assessments, day care, equipment and home adaptations and meals for the period FYE 1996 to FYE 2014; and short-term care to maximise independence from FYE 2015 to FYE 2017.
- For FYE 2015, productivity is not estimated due to a break in series.
Download this chart Figure 14: Quality and non-quality adjusted productivity for directly-measured ASC services only and all ASC services, FYE 1997 to FYE 2018
Image .csv .xlsFigure 14 shows that productivity for directly measured ASC services declined by more than the overall productivity measure for all ASC services. This is due to the inclusion of the indirectly measured component reducing the scale of productivity changes in the overall measure.
This effect is more noticeable after FYE 2015, when the indirectly measured component increased to around two-thirds of total public ASC expenditure. Between FYE 2015 and FYE 2018, non-quality adjusted productivity fell by 1.8% for the overall measure but fell by 5.0% for directly measured services only.
When removing the “output-equals-inputs” component of output, which experienced a largely positive quality adjustment during the final three years of the series, quality adjusted productivity fell by 4.4% for directly measured services, compared with a fall of 0.5% for the overall measure.
In contrast to the overall productivity measure, the directly measured productivity measure indicates that ASC productivity may be falling faster after FYE 2015 than the relatively stable period of FYE 2010 to FYE 2014. However, comparisons of productivity growth between these two periods are complicated by changes in the types of service covered. As shown in Section 10, residential and nursing care, which makes up most of directly measured output after FYE 2015, had lower productivity in FYE 2014 than at the start of the series. In contrast, community care productivity, which was included on a directly measured basis before FYE 2014, was at a similar level in FYE 2014 as in FYE 1997.
Back to table of contents9. Productivity by client age group
This section analyses the productivity of adult social care (ASC) services by the two main client age group classifications used by NHS Digital: working age adults (those aged 18 to 64 years) and older adults (those aged 65 years and over).
The reasons older adults and working age adults need social care support often differ. In FYE 2018, the majority of ASC expenditure on older adults was to provide support for physical disabilities, while the majority of ASC expenditure on working age adults was to provide support for learning disabilities.
Figure 15, 16 and 17 show, respectively, the proportion of the overall population, proportion of local authority clients accessing long-term care and proportion of public expenditure on ASC that each client age group accounts for.
Figure 15: Adult population by age group, mid-2017
England
Source: Office for National Statistics
Download this chart Figure 15: Adult population by age group, mid-2017
Image .csv .xlsFigure 16: Number of clients accessing local authority-provided or -arranged long term support at year-end by age group, FYE 2018
England
Source: Office for National Statistics
Notes:
- Long-term support accounts for the majority of adult social care expenditure, but does not include short-term support.
Download this chart Figure 16: Number of clients accessing local authority-provided or -arranged long term support at year-end by age group, FYE 2018
Image .csv .xlsFigure 17: Public expenditure on adult social care by age group, FYE 2018
England
Source: Office for National Statistics
Notes:
- Includes only expenditure which can be attributed to a specific age group.
Download this chart Figure 17: Public expenditure on adult social care by age group, FYE 2018
Image .csv .xlsFigures 15 and 16 show that, while working age adults make up 77% of the adult population in England, they account for only 40% of clients accessing long-term support.
However, Figure 17 shows that of public expenditure on ASC services which can be attributed to a specific age group1 , 53% of public spending on ASC services funded care for working age adults and 47% was spent on older adults in financial year ending (FYE) 2018. As a result, public adult social care expenditure per adult receiving long-term support is higher for working age adults than older adults.
Reasons for the difference in the proportion of long-term clients who are working age and the proportion of public ASC expenditure on working age adults, include the higher cost-per-week of providing care for working age adults, particularly clients with learning disabilities, and the smaller proportion of working age clients’ costs funded by client contributions2 .
Inputs for working age adults’ care increased by 15.4% between FYE 2006 and FYE 2018, while inputs for older adults’ care decreased by 11.2%
Figure 18 shows the growth in ASC inputs for working age and older adults’ care for services which can be attributed to a specific age band.
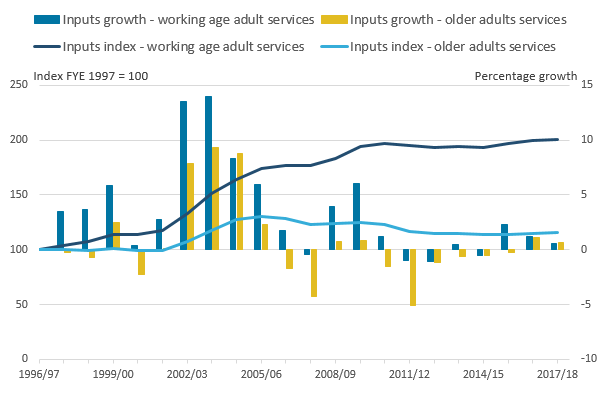
Figure 18: Public service adult social care inputs by age group, FYE 1997 to FYE 2018
England
Source: Office for National Statistics
Notes:
- The same deflators are used for the inputs of older and working age adults’ care. This may not reflect the real cost inflation of older and working age adults’ care if input inflation differs between inputs for older and working age adults’ care.
- For FYE 2015, inputs growth is not estimated separately for older and working age adults' care due to a break in series in the data source.
Download this image Figure 18: Public service adult social care inputs by age group, FYE 1997 to FYE 2018
.png (20.8 kB) .xls (29.7 kB)Figure 18 shows that while inputs for both older and working age adults’ care grew between FYE 1997 and FYE 2006, inputs for working age adults’ care grew by more than twice as much, increasing by 74% relative to 30% for older adults’ care. Since FYE 2006, inputs for older adults’ care fell by 11.2%, while inputs for working age adults’ care rose by 15.4%.
Figure 19 contrasts the productivity changes for older and working age adults. For comparability, both series measure only services for which activity data are available3 , due to the methodological issues mentioned in Section 8.
Figure 19: Quality and non-quality adjusted productivity for older adults and working age adults, directly-measured ASC services only, FYE 1997 to FYE 2018
England
Source: Office for National Statistics
Download this chart Figure 19: Quality and non-quality adjusted productivity for older adults and working age adults, directly-measured ASC services only, FYE 1997 to FYE 2018
Image .csv .xlsFigure 19 shows that the productivity of ASC for working age adults’ fell by more than that that of older adults. This divergence occurred between FYE 1997 and FYE 2011 as the productivity for older adults’ care fell by 10.6% and the productivity for working age adults’ care fell by 29.4%.
This divergent performance may be related to increases in the intensity of care, which could be due to a focus on more intensive care for working age adults or a reduction in service provision for working age adults with lower needs. However, as the Adult Social Care Survey did not exist in the years over which the main divergence in productivity occurred, it is not possible to measure changes in needs or service quality for the different groups. It should also be noted that the same deflators are applied to the inputs for both age groups and this may be a source of some of the difference in these productivity series, as the higher cost of services for adults with learning disabilities is due partly to their more labour-intensive nature.
Since FYE 2011, this trend has reversed, with non-quality adjusted productivity falling by 10.3% for older adults’ care between FYE 2011 and FYE 2018 but by only 3.4% working age adults. In addition, the quality adjustment for working age adults’ care grew more strongly over the same period, increasing by 4.3% relative to 2.5% for older adults’ care. As a result, quality adjusted productivity rose for working age adults’ care between FYE 2011 and FYE 2018, while productivity for older adults’ care fell.
Notes for: Productivity by client age group
- Not all ASC expenditure can be attributed to a specific age group. In FYE 2018, 24% of public expenditure on ASC was not attributable to specific age groups, including expenditure on commissioning and service delivery, and information and early intervention.
- As both the inputs and output series used to measure productivity are adjusted to remove client contributions, changes in client contributions do not affect the productivity measure.
- Services for which output is measured directly and by age band are: residential and nursing care for the whole series; day care and referrals and assessments until FYE 2014; and short-term care to maximise independence from FYE 2015 to FYE 2017.
10. Productivity by service type
Figure 20 shows the proportion of public adult social care (ASC) expenditure made up by each service type and how this has changed over time.
Figure 20: Public expenditure on adult social care by service type, FYE 1997 to FYE 2018
England
Source: Office for National Statistics
Notes:
- Expenditure on direct payments was first separately recorded in the data in FYE 2001.
- There is a break in series between FYE 2014 and FYE 2015 due to a change of data collection, resulting in most community services being measured indirectly from FYE 2015 on, and so are included in the other ASC expenditure category from FYE 2015 on.
- Other ASC expenditure included meals, equipment and adaptations, as well as indirectly measured services other than direct payments. From FYE 2015, this category additionally includes most community services, including short-term care to maximise independence.
- Sum of components of adult social care expenditure might not add up to 100 due to rounding.
Download this chart Figure 20: Public expenditure on adult social care by service type, FYE 1997 to FYE 2018
Image .csv .xlsFigure 20 shows that residential and nursing care accounted for 45% of public ASC expenditure in financial year ending (FYE) 1997, but this had fallen to 32% in FYE 2018. In contrast, direct payments increased from 0.6% of expenditure when this was first recorded in FYE 2001, to 10.1% in FYE 2018.
This section analyses ASC productivity by three broad service types measured using the preferred directly-measured output methodology. These are: residential and nursing care; community care, which includes home care, day care and other directly-measured services; and referrals and assessments.
Residential and nursing care is the only service type to be measured using the preferred directly measured output methodology throughout the series, with the exception for FYE 2015, when there was a change in data collection.
Residential and nursing care output is measured by the number of weeks of care provided, with different weights given to different client age and support need groups, to account for differences in the cost of providing care to different client groups.
Residential and nursing care productivity fell by 1.8% in FYE 2018 as inputs fell 0.3% but quality adjusted output fell by 2.1%
Figure 21: Public service residential and nursing care; inputs, and quality adjusted and non-quality adjusted output and productivity, FYE 1997 to FYE 2018
England
Source: Office for National Statistics
Download this chart Figure 21: Public service residential and nursing care; inputs, and quality adjusted and non-quality adjusted output and productivity, FYE 1997 to FYE 2018
Image .csv .xlsFigure 21 shows that publicly funded residential and nursing care output grew between FYE 1997 and FYE 2005 but fell in every year since. In FYE 2018, output fell to a level below that of the start of the series in FYE 1997.
Residential and nursing care productivity declined by 19.1% between its peak in FYE 2002 and FYE 2010. Residential and nursing care productivity experienced almost no change between FYE 2010 and FYE 2014 as output and inputs fell at the same rate. However, between FYE 2015 and FYE 2018, inputs have fallen by only 0.4% while quality-adjusted output fell by 3.8%, resulting in a productivity fall of 3.4%.
The quality adjustment added 0.7% to output between FYE 2011 and FYE 2018, although this increase was not continuous with quality falling in FYE 2014 and FYE 2018.
For community care, quality adjusted productivity increased by 2.4% over the three years this measure was available, FYE 2011 to FYE 2014
Figure 22 shows inputs, output and productivity for community care services. These include home care, day care, equipment and home adaptations, and “meals-on-wheels”. The activity data collection for all of these services ended in FYE 2014, so it is not possible to observe more recent productivity trends.
Figure 22: Public service community adult social care; inputs, and quality adjusted and non-quality adjusted output and productivity, FYE 1997 to FYE 2014
England
Source: Office for National Statistics
Download this chart Figure 22: Public service community adult social care; inputs, and quality adjusted and non-quality adjusted output and productivity, FYE 1997 to FYE 2014
Image .csv .xlsFigure 22 shows that community adult social care (ASC) services experienced strong growth in inputs and output more recently than residential and nursing care, with output peaking in FYE 2009 and inputs peaking in FYE 2011, both at more than 30% higher than the level in FYE 1997.
Between FYE 2011 and FYE 2014, quality adjusted productivity increased by 2.4% with the quality adjustment adding 6.0% to productivity. While this suggests greater improvements in the quality of community ASC services than residential and nursing care services, although it should be noted that different methodologies are used to produce the quality adjustment for residential and nursing care, and for community care.
Figures 22 also shows that community care did not experience the same steady fall in productivity as residential and nursing care providers. It should also be noted that as no specific deflators are available for capital expenditure, this element of inputs is not calculated separately by service type. If there are large differences in capital consumption expenditure or inflation between residential and nursing care and community care, this could account for some of the difference between the two series.
More information on the methodological differences can be found in Public service productivity: adult social care, current method, 2019 update.
The output of ASC referrals and assessments was 2.7% lower in FYE 2014 than FYE 1997, despite a 45.3% increase in inputs
Figure 23 shows the final and smallest element of directly measured output, referrals to local authority (LA) social care services and assessments to determine what care would be appropriate for clients. Due to no specific quality adjustment being available for referrals and assessments, only non-quality adjusted productivity is displayed for this measure.
Figure 23: Referrals and assessments for adult social care; inputs, non-quality adjusted output and productivity, FYE 1997 to FYE 2014
England
Source: Office for National Statistics
Download this chart Figure 23: Referrals and assessments for adult social care; inputs, non-quality adjusted output and productivity, FYE 1997 to FYE 2014
Image .csv .xlsThe productivity of referrals and assessment services declined by 34.6% between FYE 1997 and FYE 2006 as inputs rose. This fall in productivity could be as a result of more thorough or complex assessments taking place but the lack of quality data for this service do not enable us to measure this. Changes to inputs, output and productivity since FYE 2006 are more minor with all three at similar levels at the end of the series in FYE 2014 than they were in FYE 2006.
Back to table of contents11. Revisions
Figure 24 shows how the adult social care (ASC) productivity series has been revised since the first ONS ASC productivity figures for England were published in Measuring adult social care productivity in the UK and England.
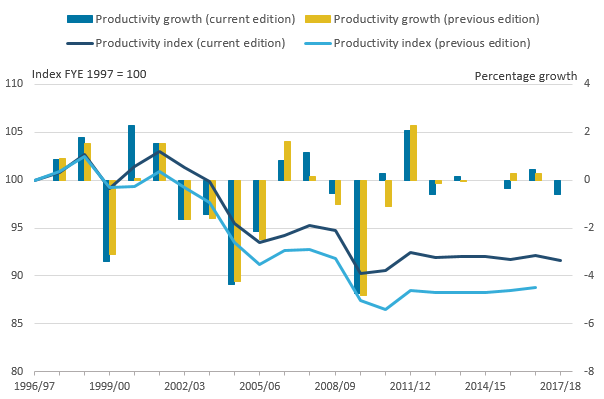
Figure 24: Revisions to public service adult social care productivity, FYE 1997 to FYE 2017
England
Source: Office for National Statistics
Notes:
- Quality adjustment applies after financial year ending 2011.
Download this image Figure 24: Revisions to public service adult social care productivity, FYE 1997 to FYE 2017
.png (24.5 kB) .xls (28.7 kB)One of the main causes of difference between the new series and previously published series is the adoption of a new set of deflators for labour costs. These are produced by the Department of Health and Social Care and the revision is due to a change in data source from the Annual Survey of Hours and Earnings to the National Minimum Data Set for Social Care.
The series is also affected by a methodological improvement for financial year ending (FYE) 2001 to better align the inputs and output for some of the smaller service types, including equipment and adaptations and meals. This increases output growth in FYE 2001 and therefore raises the productivity index for subsequent years.
A further change was the disaggregation of older adults’ residential and nursing care by primary support need for the years FYE 2015 onwards, to better reflect differences in the cost of care for different client groups. This data is not available for earlier years.
Back to table of contents