Table of contents
- Main points
- Things you need to know about this release
- How have we defined avoidable mortality?
- Avoidable mortality rates for the UK and constituent countries by sex and cause
- Amenable mortality rates for the UK and constituent countries by sex and cause
- Preventable mortality rates for the UK and constituent countries by sex and cause
- Avoidable mortality rates for sub-national areas in England and Wales
- Avoidable mortality in children and young people for the UK and constituent countries by sex and cause
- Concept of avoidable mortality
- Quality and methodology
1. Main points
In 2016, approximately 24% of all deaths in the UK were considered avoidable (141,101 deaths out of 597,206).
Scotland had the highest rate of avoidable deaths for males and females compared with the other constituent countries of the UK, whereas England had the lowest rate.
In 2016, deaths from neoplasms (cancers and other non-cancerous tissue growths) continued to be the leading cause of avoidable deaths in the UK.
Amenable mortality in the UK has significantly increased since 2014 with 123.2 amenable deaths per 100,000 persons in 2016.
For females in England, the local authorities with the five highest avoidable mortality rates were all located in the three northernmost regions.
For males in Wales, the highest avoidable mortality rate was in Merthyr Tydfil local authority at 384.4 deaths per 100,000, an additional 152 deaths per 100,000 than in Monmouthshire, which had the lowest rate at 232.4 deaths per 100,000.
Amongst children and young people (aged 0 to 19 years) 34% of all deaths in the UK were considered avoidable in 2016.
The highest number of avoidable deaths in children and young people in the UK in 2016 were from maternal and infant causes.
2. Things you need to know about this release
Previously the avoidable mortality bulletin presented avoidable deaths for England and Wales. To increase usability, the coverage of this bulletin has been widened to represent avoidable mortality in the UK. Figures for the UK are calculated using death registration data for England and Wales held by Office for National Statistics (ONS) and death registration data for Scotland and Northern Ireland kindly provided by National Records of Scotland and the Northern Ireland Statistics and Research Agency respectively.
Figures in this release are presented for causes of death that are considered avoidable in the presence of timely and effective healthcare or public health interventions (avoidable mortality).
While a particular condition can be considered avoidable, this doesn’t mean that every death from that condition could be averted. This is because factors such as the lifestyle and age of the patient, the extent of disease progression at diagnosis and the potential existence of other medical conditions are not taken into account when making a list of causes.
For most of the causes of death included in our definition there is an upper age limit of 74 years. This is because deaths at older ages are often difficult to attribute definitively to a single underlying cause and the chances of death are more affected by coexisting medical conditions and other factors.
It is widely accepted that the contribution of healthcare to improvements in population health ought to be quantified. Avoidable mortality, which is based on the concept that premature deaths from certain conditions should be rare and ideally should not occur in the presence of timely and effective healthcare, is used as an indicator to measure this contribution.
Avoidable mortality was not intended to serve as a definitive source of evidence of differences in effectiveness of healthcare systems. It was designed to highlight areas of potential weaknesses in healthcare that could benefit from further in-depth investigation. Therefore, a degree of caution is recommended when interpreting the data. Further information about the limitations of the concept of avoidable mortality is available in the avoidable mortality quality and methodology information report.
With advances in medical technology and wider public health interventions, deaths from a condition which was previously not avoidable may have since become avoidable. This means that when the list of avoidable causes of death is updated, it may not be appropriate to produce previously published data using the revised avoidable mortality definition. For this reason, data presented in this bulletin are from 2014 onwards – the data year in which we implemented the revised definition. Where comparisons with the most recent available data are discussed in the bulletin, these should not be interpreted as long-term trends as differences may be due to year-on-year fluctuation. Previously published data before 2014 have not been reproduced using the revised avoidable mortality definition.
In addition to reporting age-standardised rates of avoidable mortality, standardised years of life lost (SYLL) was calculated for England and Wales only. This indicator is a measure of the potential number of years lost when a person dies prematurely from an avoidable cause. This data can be found in the accompanying datasets.
Update: 29 October 2018
In the compilation of avoidable mortality statistics, we have sought the views of government bodies regarding their usefulness for policy and service delivery. Considering the views assembled, we extended the coverage of the avoidable mortality publications to Scotland and Northern Ireland to enable a UK measure to be estimated. We also extended these measures to sub-national areas of England and Wales, including health bodies, to identify specific parts of England and Wales with higher than average avoidable deaths, and to area deprivation groupings to estimate the trend in the socioeconomic inequality.
We provide early access for quality assurance to a small number of people working in other government bodies. This is to acknowledge use of mortality data we do not own, in the case of Scotland and Northern Ireland, and for general comment on the plausibility of our findings. However, ONS itself independently produces these statistics, including determining the focus, content, commentary, illustration and interpretation of these measures presented in bulletins.
Update: 16 January 2019
We would like to clarify that our definition of avoidable mortality is different to the measure of avoidable deaths in hospital NHS trusts are required to publish figures on. We use a defined set of underlying causes of death that have been approved through consultation with users and expert guidance. It includes conditions where it is reasonable to expect deaths to be avoided through good quality healthcare, even after the condition has developed (amenable mortality), as well as those where it is possible to prevent the condition from occurring in the first place (incidence reduction) through wider public health interventions, such as those targeted at reducing the incidence of smoking (preventable mortality). The avoidable deaths in hospital measure is based on a record review of a sample of deaths deemed to be due to problems in care. Avoidable deaths in hospital data are not intended to be comparable and are not collated centrally.
Back to table of contents3. How have we defined avoidable mortality?
Amenable mortality:
- a death is amenable (treatable) if, in the light of medical knowledge and technology available at the time of death, all or most deaths from that cause (subject to age limits if appropriate) could be avoided through good quality healthcare
Preventable mortality:
- a death is preventable if, in the light of understanding of the determinants of health at the time of death, all or most deaths from that cause (subject to age limits if appropriate) could be avoided by public health interventions in the broadest sense
Avoidable mortality:
- avoidable deaths are all those defined as preventable, amenable (treatable) or both, where each death is counted only once; where a cause of death is both preventable and amenable, all deaths from that cause are counted in both categories when they are presented separately
4. Avoidable mortality rates for the UK and constituent countries by sex and cause
Males more likely to die from an avoidable cause than females
In 2016, approximately 24% of all deaths in the UK were from causes considered avoidable (141,101 deaths out of 597,206) with an age-standardised mortality rate of 228.7 deaths per 100,000 persons. The avoidable mortality rate for all persons in the UK had a small but significant increase from 2014 to 2015 followed by a non-significant decrease from 2015 to 2016 (Figure 1).
Of the avoidable deaths in 2016, males accounted for 60%, which remains unchanged since 2014. For males in 2016, approximately 29% of all deaths were from an avoidable cause (84,567 out of 293,001 deaths), whereas for females around 19% of all deaths were from avoidable causes (56,534 out of 304,205 deaths). This results in the male rate in 2016 being significantly higher at 285.1 deaths per 100,000 than the female rate at 176.2 deaths per 100,000.
Figure 1: Age-standardised avoidable mortality rates by sex
UK, 2014 to 2016
Source: Office for National Statistics, National Records of Scotland, Northern Ireland Statistics and Research Agency
Notes:
- Age-standardised mortality rates are expressed per 100,000 population and standardised to the 2013 European Standard Population. Age-standardised mortality rates are used to allow comparison between populations which may contain different proportions of people of different ages.
- Deaths of non-residents are included in figures for the UK.
- Figures are for deaths registered in each calendar year.
Download this chart Figure 1: Age-standardised avoidable mortality rates by sex
Image .csv .xlsAvoidable mortality rates significantly increased for males in Scotland and in Wales
There has been a marked increase in rates of avoidable mortality for males in Scotland and in Wales since 2014. The male age-standardised avoidable mortality rate in 2016 in Scotland was 376.2 deaths per 100,000, a significant increase from 2014 where the rate was 356.7 deaths per 100,000. Similarly, in Wales there was a significant increase in the male mortality rate from 300.4 deaths per 100,000 in 2014 to 323.6 deaths per 100,000 in 2016.
Avoidable mortality rates in Northern Ireland and England for males showed no statistically significant change since 2014, with rates in 2016 observed at 299.3 deaths per 100,000 in Northern Ireland and 271.7 deaths per 100,000 in England.
Figure 2: Age-standardised avoidable mortality rates by UK country
Males, 2014 to 2016
Source: Office for National Statistics, National Records of Scotland, Northern Ireland Statistics and Research Agency
Notes:
- Age-standardised mortality rates are expressed per 100,000 population and standardised to the 2013 European Standard Population. Age-standardised mortality rates are used to allow comparison between populations which may contain different proportions of people of different ages.
- Figures for England, Northern Ireland and Wales exclude deaths of non-residents. Figures for Scotland include deaths of non-residents.
- Figures are for deaths registered in each calendar year.
Download this chart Figure 2: Age-standardised avoidable mortality rates by UK country
Image .csv .xlsAvoidable mortality rates for females in Scotland between 2014 and 2016 showed a not statistically significant rise from 222.6 to 231.9 deaths per 100,000. In 2016, female mortality rates in Wales (194.3 deaths per 100,000 females), Northern Ireland (187.8 per 100,000 females) and England (168.2 deaths per 100,000 females) showed no statistically significant change since 2014.
Figure 3: Age-standardised avoidable mortality rates by UK country
Females, 2014 to 2016
Source: Office for National Statistics, National Records of Scotland, Northern Ireland Statistics and Research Agency
Notes:
- Age-standardised mortality rates are expressed per 100,000 population and standardised to the 2013 European Standard Population. Age-standardised mortality rates are used to allow comparison between populations which may contain different proportions of people of different ages.
- Figures for England, Northern Ireland and Wales exclude deaths of non-residents. Figures for Scotland include deaths of non-residents.
- Figures are for deaths registered in each calendar year.
Download this chart Figure 3: Age-standardised avoidable mortality rates by UK country
Image .csv .xlsNeoplasms (cancers and other non-cancerous tissue growths) were the leading cause of avoidable deaths in the UK in 2016
Causes of avoidable mortality can be categorised into broad groups. These broad cause groups are defined as cardiovascular diseases, drug use disorders, infections, injuries (which includes unintentional and intentional injuries), neoplasms (cancers and other non-cancerous tissue growths), respiratory diseases, and other (which includes nutritional, endocrine and metabolic disorders, neurological disorders, digestive disorders, genitourinary disorders, and maternal and infant conditions). Further details of the underlying causes included in the broad groups can be found in the avoidable mortality definition in the accompanying datasets.
The leading cause of avoidable deaths for broad cause groups across the constituent countries in 2016 was neoplasms with age-standardised mortality rates ranging from 75.2 deaths per 100,000 population in England to 94.3 deaths per 100,000 population in Scotland. Since 2014, mortality rates from neoplasms have declined; however, this decline was only statistically significant for England.
In 2016, Scotland had the highest avoidable mortality rate for six out of the seven broad cause groups. For five broad cause groups, the rate was significantly higher in Scotland than in the other constituent countries; for infections, it was only significantly higher than England and Northern Ireland. Wales had the highest avoidable mortality rate from respiratory diseases in 2016 with 33.2 deaths per 100,000 population, significantly higher than England and Northern Ireland.
In contrast, the broad cause group with the lowest avoidable mortality rate in 2016 was infections, with rates ranging from 1.9 deaths per 100,000 population in Northern Ireland to 4.5 deaths per 100,000 population in Scotland. Mortality rates for infections have remained relatively constant since 2014 for all the constituent countries.
Figure 4: Avoidable mortality rates by broad cause group
UK, 2016
Source: Office for National Statistics, National Records of Scotland, Northern Ireland Statistics and Research Agency
Notes:
- Age-standardised mortality rates are expressed per 100,000 population and standardised to the 2013 European Standard Population. Age-standardised mortality rates are used to allow comparison between populations which may contain different proportions of people of different ages.
- Figures for England, Northern Ireland and Wales exclude deaths of non-residents. Figures for Scotland include deaths of non-residents.
- Figures are for deaths registered in the calendar year 2016
- The "Other" cause group consists of nutritional, endocrine and metabolic disorders, neurological disorders, digestive disorders, genitourinary disorders, and maternal and infant conditions.
- See accompanying datasets for further details of the underlying causes of death included in the avoidable mortality definition.
Download this chart Figure 4: Avoidable mortality rates by broad cause group
Image .csv .xlsFor England and Wales only, broad cause groups were broken down further into specific causes of death to observe their impact on avoidable mortality. In 2016, the specific cause with the highest number of avoidable deaths in England and in Wales was ischaemic heart disease (IHD) accounting for 16% of all avoidable deaths in England (17,922 out of 112,406 avoidable deaths) and 17% of all avoidable deaths in Wales (1,392 out of 8,132 avoidable deaths). Given the high number of avoidable deaths from IHD, it can become difficult to assess the contribution of other causes of death groupings to avoidable mortality. It is likely that any change in avoidable mortality figures will be heavily influenced by changes in the number of deaths from IHD. For this reason, avoidable, amenable and preventable mortality data excluding IHD have been calculated for England and Wales and can be found in the accompanying datasets.
Back to table of contents5. Amenable mortality rates for the UK and constituent countries by sex and cause
Amenable mortality rates in the UK have significantly increased since 2014
There were 75,736 deaths from causes considered amenable to healthcare in the UK in 2016, an age-standardised rate of 123.2 deaths per 100,000 population. This has significantly increased since 2014 when there were 71,656 amenable deaths and an age-standardised rate of 121.3 deaths per 100,000 population.
Amenable mortality rates for males and females in Scotland, England and Wales all increased from 2014 to 2016. The largest increases were observed in Wales and Scotland, where male amenable mortality rates increased by 6% and 4% respectively and female amenable mortality rates increased by 8% and 6% respectively. Decreases in amenable mortality rates were observed in Northern Ireland, but these were modest at less than 1%. However, all the observations across the four constituent countries were not statistically significant.
Cardiovascular diseases were the leading cause of amenable deaths in the UK
The leading cause of amenable mortality in 2016 was cardiovascular diseases, accounting for between 42% (England and Northern Ireland) and 45% (Scotland) of all deaths amenable to healthcare across the constituent countries. Mortality rates for cardiovascular diseases ranged from 50.3 deaths per 100,000 population in England to 68.8 deaths per 100,000 population in Scotland. Since 2014, mortality rates across the four constituent countries have remained at a similar level.
Respiratory diseases accounted for 24% of all deaths amenable to healthcare in Wales in 2016 making it the second-highest amenable cause of death for the country with a mortality rate of 33.2 deaths per 100,000 population. In comparison, neoplasms (cancers and other non-cancerous tissue growths) was the second-highest cause in Scotland, Northern Ireland and England with mortality rates ranging from 27.7 deaths per 100,000 in England to 31.3 deaths per 100,000 population in Scotland.
In Northern Ireland the cause group with the lowest mortality rate was infections, where there were 1.9 deaths per 100,000 population compared with the other constituent countries whose lowest rates were from injuries.
Figure 5: Amenable mortality rates by broad cause group
UK, 2016
Source: Office for National Statistics, National Records of Scotland, Northern Ireland Statistics and Research Agency
Notes:
- Age-standardised mortality rates are expressed per 100,000 population and standardised to the 2013 European Standard Population. Age-standardised mortality rates are used to allow comparison between populations which may contain different proportions of people of different ages.
- Figures for England, Northern Ireland and Wales exclude deaths of non-residents. Figures for Scotland include deaths of non-residents.
- Figures are for deaths registered in the calendar year 2016
- The "Other" cause group consists of nutritional, endocrine and metabolic disorders, neurological disorders, digestive disorders, genitourinary disorders, and maternal and infant conditions.
- See accompanying datasets for further details of the underlying causes of death included in the avoidable mortality definition.
Download this chart Figure 5: Amenable mortality rates by broad cause group
Image .csv .xls6. Preventable mortality rates for the UK and constituent countries by sex and cause
Preventable mortality rates significantly increased for males in Scotland and Wales
There were 117,840 deaths that were considered preventable through wider public health interventions in the UK in 2016; an age-standardised rate of 191.0 deaths per 100,000 population. In 2014 there were 113,418 preventable deaths and a rate of 190.6 deaths per 100,000 population; this slight increase in rate was not statistically significant.
There were statistically significant increases in preventable mortality rates between 2014 and 2016 among males, rising by 5% in Scotland and 9% in Wales. Female rates also increased by 3% for both Scotland and Wales; however, these increases were not statistically significant. Preventable mortality rates for both sexes in England and Northern Ireland have remained relatively stable since 2014.
Neoplasms (cancers and other non-cancerous tissue growths) caused between 36% and 40% of all deaths from preventable conditions
The leading cause of preventable mortality in 2016 was neoplasms (cancers and other non-cancerous tissue growths), which accounted for between 36% (Scotland) and 40% (Northern Ireland) of all preventable deaths, with mortality rates ranging from 71.4 deaths per 100,000 population in England and 89.7 deaths per 100,000 population in Scotland. Since 2014, preventable mortality rates from neoplasms have steadily decreased.
Injuries (including both intentional and unintentional injuries) was the second leading cause of preventable mortality in 2016 for Scotland and Northern Ireland, with observed increases since 2014 of 18% and 10% respectively. These changes reflect trends reported in our statistical bulletin for suicides in the UK (however, suicide is defined differently across the two bulletins). In contrast, cardiovascular diseases was the second leading cause of preventable mortality in 2016 for England and for Wales.
Figure 6: Preventable mortality rates by broad cause group
UK, 2016
Source: Office for National Statistics, National Records of Scotland, Northern Ireland Statistics and Research Agency
Notes:
- Age-standardised mortality rates are expressed per 100,000 population and standardised to the 2013 European Standard Population. Age-standardised mortality rates are used to allow comparison between populations which may contain different proportions of people of different ages.
- Figures for England, Northern Ireland and Wales exclude deaths of non-residents. Figures for Scotland include deaths of non-residents.
- Figures are for deaths registered in the calendar year 2016
- The "Other" cause group consists of nutritional, endocrine and metabolic disorders, neurological disorders, digestive disorders, genitourinary disorders, and maternal and infant conditions.
- Northern Ireland infections data are not included as age-standardised mortality rates based on fewer than 10 deaths are not calculated owing to low reliability.
- See accompanying datasets for further details of the underlying causes of death included in the avoidable mortality definition.
Download this chart Figure 6: Preventable mortality rates by broad cause group
Image .csv .xls7. Avoidable mortality rates for sub-national areas in England and Wales
Mortality rates generally higher in the north, particularly in Manchester, during 2014 to 2016
For males, of the 324 local authorities in England, avoidable mortality was highest in Manchester with an age-standardised mortality rate of 481.2 deaths per 100,000 males, which was more than 200 additional deaths per 100,000 males compared with England over these years. Of the five local authorities with the highest avoidable mortality rates, three were located in the North West region of England and one was located in the North East region (Table 1). In contrast, the five lowest avoidable mortality rates were found in county districts in the three southernmost regions excluding London. Avoidable mortality for males was close to three times higher in Manchester than East Dorset, with an extra 311 avoidable deaths per 100,000 in this northern city.
For females the north-south divide was even clearer, with the five highest avoidable mortality rates all located in the three northern regions. Although avoidable mortality is generally higher for males, Manchester’s females had a statistically significantly higher avoidable mortality rate than males in more than half of the local authorities in England.
Table 1: Age-standardised avoidable mortality rates for the highest- and lowest-ranked local authorities in England by sex, 2014 to 2016
| Males | Females | |||||||
|---|---|---|---|---|---|---|---|---|
| Local Authority | Mortality rate per 100,000 population | Rank | Local Authority | Mortality rate per 100,000 population | Rank | |||
| Manchester | 481.2 | 1 | Manchester | 304.1 | 1 | |||
| Blackpool | 471.8 | 2 | −−− | Blackpool | 281.7 | −− | 2 | |
| Corby | 428.1 | 3 | Middlesbrough | 276.9 | 3 | |||
| Middlesbrough | 413.8 | 4 | −−− | Knowsley | 272.5 | −− | 4 | |
| Liverpool | 404.4 | 5 | −−− | Kingston upon Hull, City of | 264.9 | 5 | ||
| Surrey Heath | 180.0 | 320 | Hart | 113.1 | −− | 320 | ||
| Chiltern | 177.0 | 321 | −−− | East Hertfordshire | 112.8 | 321 | ||
| Hart | 174.0 | 322 | South Cambridgeshire | 110.1 | −− | 322 | ||
| South Cambridgeshire | 173.1 | 323 | −−− | South Oxfordshire | 106.4 | 323 | ||
| East Dorset | 170.2 | 324 | Chiltern | 103.2 | −− | 324 | ||
| Source: Office for National Statistics | ||||||||
| Notes: | ||||||||
| 1. Age-standardised mortality rates are expressed per 100,000 population and standardised to the 2013 European Standard Population. Age-standardised mortality rates are used to allow comparison between populations which may contain different proportions of people of different ages. | ||||||||
| 2. Figures for England exclude deaths of non-residents. | ||||||||
| 3. Figures are for deaths registered in the calendar years 2014 to 2016. | ||||||||
Download this table Table 1: Age-standardised avoidable mortality rates for the highest- and lowest-ranked local authorities in England by sex, 2014 to 2016
.xls (38.9 kB)Merthyr Tydfil had highest avoidable mortality rates across local authorities in Wales
In Wales the variation in avoidable mortality across the 22 local authorities was substantially smaller than in England over the period 2014 to 2016. However, those local authorities with the highest rates were located in the former heavy industrial centres, while the lowest were found in rural parts of Wales.
For males, the highest avoidable mortality rate was observed in Merthyr Tydfil local authority at 384.4 deaths per 100,000, an additional 152 deaths per 100,000 than in Monmouthshire, which had the lowest rate at 232.4 deaths per 100,000.
For females, avoidable mortality rates were also highest in Merthyr Tydfil at 255.9 deaths per 100,000 females, but lowest in Powys at 144.0 deaths per 100,000 females. The five local authorities with the lowest and highest rates were the same for both males and females (Table 2).
Table 2: Age-standardised avoidable mortality rates for the highest- and lowest-ranked local authorities in Wales by sex, 2014 to 2016
| Males | Females | |||||||
|---|---|---|---|---|---|---|---|---|
| Local Authority | Mortality rate per 100,000 population | Rank | Local Authority | Mortality rate per 100,000 population | Rank | |||
| Merthyr Tydfil | 384.4 | 1 | Merthyr Tydfil | 255.9 | 1 | |||
| Blaenau Gwent | −−− | 364.5 | 2 | −−−− | Blaenau Gwent | −−− | 234.2 | 2 |
| Rhondda Cynon Taf | −−− | 364.2 | 3 | Rhondda Cynon Taf | −−− | 227.0 | 3 | |
| Neath Port Talbot | 360.8 | 4 | Caerphilly | 226.3 | 4 | |||
| Caerphilly | −−− | 343.1 | 5 | −−−− | Neath Port Talbot | 215.3 | 5 | |
| Pembrokeshire | 277.5 | 18 | Pembrokeshire | −−− | 166.1 | 18 | ||
| Vale of Glamorgan | 267.2 | 19 | −−−− | Vale of Glamorgan | 163.8 | 19 | ||
| Ceredigion | −−− | 266.7 | 20 | Monmouthshire | −−− | 163.6 | 20 | |
| Powys | −−− | 259.7 | 21 | −−−− | Ceredigion | 157.4 | 21 | |
| Monmouthshire | 232.4 | 22 | Powys | 144.0 | 22 | |||
| Source: Office for National Statistics | ||||||||
| Notes: | ||||||||
| 1. Age-standardised mortality rates are expressed per 100,000 population and standardised to the 2013 European Standard Population. Age-standardised mortality rates are used to allow comparison between populations which may contain different proportions of people of different ages. | ||||||||
| 2. Figures for Wales exclude deaths of non-residents. | ||||||||
| 3. Figures are for deaths registered in the calendar years 2014 to 2016. | ||||||||
Download this table Table 2: Age-standardised avoidable mortality rates for the highest- and lowest-ranked local authorities in Wales by sex, 2014 to 2016
.xls (38.4 kB)Figure 7: Age-standardised avoidable mortality rates by local authority in England and Wales by sex, 2014 to 2016
Embed code
Amenable mortality for males more than four times higher in NHS Bradford City than in NHS Richmond
NHS Bradford City had the highest rate of amenable mortality for males among England’s 207 Clinical Commissioning Groups (CCGs) in 2016. The mortality rate was significantly higher than all other CCGs (except for NHS Manchester) and was more than 2.5 times higher than the England rate. The lowest mortality rates in males were found in CCGs servicing South East England including London. One explanation for NHS Bradford City’s substantially higher rate is the fact that the population it serves is ranked as the most deprived CCG (Excel 191KB) in England. NHS Manchester, NHS Nottingham City and NHS Blackburn with Darwin are also ranked among the 20 most deprived CCGs and incidentally are located in the North West and East Midlands regions. However, NHS South Reading, which is located in the South East region, was somewhat less deprived but was among the five CCGs with the highest amenable mortality rates.
For females, amenable mortality was worse in northern CCGs generally; among the five with the highest rates, three were in North West England. NHS Manchester had the highest rate of amenable deaths, approaching twice as high as the England rate and more than three times higher than NHS Newbury and District. There were no northern populations in the five CCGs with the lowest rates.
Table 3: Age-standardised amenable mortality rates for the highest- and lowest-ranked Clinical Commissioning Groups (CCGs) in England by sex, 2016
| Males | Females | |||||
|---|---|---|---|---|---|---|
| CCGs | Mortality rate per 100,000 population | Rank | CCGs | Mortality rate per 100,000 population | Rank | |
| NHS Bradford City | 386.4 | 1 | NHS Manchester | 186.6 | 1 | |
| NHS Manchester | 267.3 | 2 | −−− | NHS Bradford City | 185.4 | 2 |
| NHS Blackburn with Darwen | 242.9 | 3 | −−− | NHS Knowsley | 163.1 | 3 |
| NHS Nottingham City | 236.3 | 4 | NHS South Tees | 153.5 | 4 | |
| NHS South Reading | 225.9 | 5 | −−− | NHS Blackpool | 153.0 | 5 |
| NHS North East Hampshire and Farnham | 96.1 | 203 | −−− | NHS Surrey Downs | 68.0 | 203 |
| NHS Chiltern | 94.3 | 204 | −−− | NHS South Gloucestershire | 65.1 | 204 |
| NHS West Hampshire | 92.5 | 205 | NHS Windsor, Ascot and Maidenhead | 64.7 | 205 | |
| NHS High Weald Lewes Havens | 92.3 | 206 | −−− | NHS Barnet | 64.1 | 206 |
| NHS Richmond | 91.1 | 207 | NHS Newbury and District | 60.9 | 207 | |
| Source: Office for National Statistics | ||||||
| 1. Age-standardised mortality rates are expressed per 100,000 population and standardised to the 2013 European Standard Population. Age-standardised mortality rates are used to allow comparison between populations which may contain different proportions of people of different ages. | ||||||
| 2. Figures for England exclude deaths of non-residents. | ||||||
| 3. Figures are for deaths registered in the calendar year 2016. | ||||||
Download this table Table 3: Age-standardised amenable mortality rates for the highest- and lowest-ranked Clinical Commissioning Groups (CCGs) in England by sex, 2016
.xls (38.4 kB)Cwm Taf University had highest amenable mortality rates across Welsh Health Boards
Across the seven Welsh Health Boards, Cwm Taf University had the highest rate of amenable mortality for both males and females, while Powys Teaching Health Board had the lowest. For males, only Powys Teaching had a statistically significant lower rate than the Wales estimate of 164.5 deaths per 100,000 males (Table 4). For females, both Powys Teaching and Hywel Dda University had statistically significantly lower amenable mortality rates compared with Wales, while Cwm Taf University had a significantly higher rate.
Table 4: Age-standardised amenable mortality rates for the highest-ranked health boards in Wales by sex, 2016
| Males | Females | |||||
|---|---|---|---|---|---|---|
| Health Boards | Mortality rate per 100,000 population | Rank | Health Boards | Mortality rate per 100,000 population | Rank | |
| Cwm Taf University | 188.9 | 1 | Cwm Taf University | 144.4 | 1 | |
| Aneurin Bevan University | 181.1 | 2 | −−−− | Aneurin Bevan University | 129.6 | 2 |
| Betsi Cadwaladr University | 165.6 | 3 | Abertawe Bro Morgannwg University | 123.7 | 3 | |
| Abertawe Bro Morgannwg University | 163.6 | 4 | Betsi Cadwaladr University | 105.7 | 4 | |
| Cardiff and Vale University | 156.2 | 5 | Cardiff and Vale University | 104.5 | 5 | |
| Hywel Dda University | 150.1 | 6 | Hywel Dda University | 90.9 | 6 | |
| Powys Teaching | 118.7 | 7 | Powys Teaching | 77.5 | 7 | |
| Source: Office for National Statistics | ||||||
| 1. Age-standardised mortality rates are expressed per 100,000 population and standardised to the 2013 European Standard Population. Age-standardised mortality rates are used to allow comparison between populations which may contain different proportions of people of different ages. | ||||||
| 2. Figures for Wales exclude deaths of non-residents. | ||||||
| 3. Figures are for deaths registered in the calendar year 2016. | ||||||
Download this table Table 4: Age-standardised amenable mortality rates for the highest-ranked health boards in Wales by sex, 2016
.xls (37.4 kB)
Figure 8: Age-standardised amenable mortality rates for all persons by Clinical Commissioning Groups (CCGs) in England and Health Boards in Wales, 2016
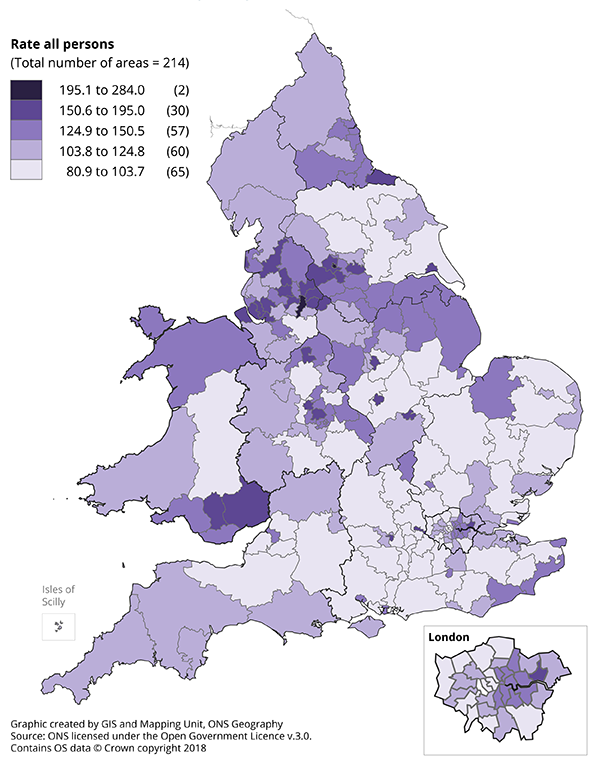
Source: Office for National Statistics
Notes:
- Age-standardised mortality rates are expressed per 100,000 population and standardised to the 2013 European Standard Population. Age-standardised mortality rates are used to allow comparison between populations which may contain different proportions of people of different ages.
- Figures exclude deaths of non-residents.
- Figures are for deaths registered in the calendar year 2016.
- Boundaries are England CCG 2017 boundaries and Wales Health Board boundaries 2016.
Download this image Figure 8: Age-standardised amenable mortality rates for all persons by Clinical Commissioning Groups (CCGs) in England and Health Boards in Wales, 2016
.png (264.2 kB) .xls (77.3 kB)8. Avoidable mortality in children and young people for the UK and constituent countries by sex and cause
34% of all deaths in children and young people in the UK were considered avoidable
In 2016, of all deaths amongst children and young people aged 0 to 19 years in the UK, 34% were from causes considered avoidable through good quality healthcare and wider public health interventions (1,674 deaths out of 4,995 deaths). Overall, avoidable deaths in children and young people made up 1% of the total number of avoidable deaths.
Of the avoidable deaths in children and young people in the UK in 2016, males accounted for almost two-thirds (61% or 1,018 deaths out of 1,674 deaths), demonstrating the higher risk faced by males in this age category. The mortality rate for males was significantly higher at 12.7 deaths per 100,000 compared with females at 8.4 deaths per 100,000. Since 2014, mortality rates have decreased with an 11% fall in avoidable deaths in males and a 2% fall in females, although these decreases were not significant.
Since 2014, Northern Ireland accounted for the highest rate of male avoidable deaths in children and young people. However, this rate has decreased by 28% from 32.6 deaths per 100,000 males to 23.6 deaths per 100,000 males in 2016. Scotland and England have also experienced decreases of 12% and 10% respectively across the three years. Wales avoidable mortality rates on the other hand have consistently increased since 2014 from 11.7 deaths per 100,000 males to 15.0 deaths per 100,000 males. However, all changes observed across the constituent countries were not statistically significant.
Figure 9: Age-standardised avoidable mortality rates by UK country for children and young people (aged 0 to 19 years)
Males, 2014 to 2016
Source: Office for National Statistics, National Records of Scotland, Northern Ireland Statistics and Research Agency
Notes:
- Age-standardised mortality rates are expressed per 100,000 population and standardised to the 2013 European Standard Population. Age-standardised mortality rates are used to allow comparison between populations which may contain different proportions of people of different ages.
- Figures for England, Northern Ireland and Wales exclude deaths of non-residents. Figures for Scotland include deaths of non-residents.
- Figures are for deaths registered in each calendar year.
Download this chart Figure 9: Age-standardised avoidable mortality rates by UK country for children and young people (aged 0 to 19 years)
Image .csv .xlsEven though the mortality rate for Scotland females decreased from 2014 to 2015, an overall increase of 27% was observed from 2014 to 2016. This led it to have the highest mortality rate for females compared with the other constituent countries of the UK in 2016. Similarly, mortality rates in Northern Ireland increased by 14% from 15.5 deaths per 100,000 females in 2014 to 17.7 deaths per 100,000 females in 2016. However, both changes were not statistically significant. England and Wales mortality rates for female children and young people have remained similar since 2014 and in 2016, their rates were significantly lower than those in Scotland and Northern Ireland.
Figure 10: Age-standardised avoidable mortality rates by UK country for children and young people (aged 0 to 19 years)
Females, 2014 to 2016
Source: Office for National Statistics, National Records of Scotland, Northern Ireland Statistics and Research Agency
Notes:
- Age-standardised rates are expressed per 100,000 population and standardised to the 2013 European Standard Population. Age-standardised rates are used to allow comparison between populations which may contain different proportions of people of different ages.
- Figures for England, Northern Ireland and Wales exclude deaths of non-residents. Figures for Scotland include deaths of non-residents.
- Figures are for deaths registered in each calendar year.
Download this chart Figure 10: Age-standardised avoidable mortality rates by UK country for children and young people (aged 0 to 19 years)
Image .csv .xlsDecreases observed in the top five leading causes of death in children and young people
From 2014 to 2016, the leading cause of avoidable deaths for children and young people in the UK was maternal and infant causes (which comprises deaths from complications of the perinatal period, congenital malformations of the circulatory system and spina bifida). Since 2014, deaths resulting from these causes have steadily decreased from 532 deaths to 470 deaths in 2016, a fall of 12%.
Decreases were also observed in unintentional injuries and intentional injuries, which also account for a large proportion of avoidable deaths in children and young people with the number of deaths in 2016 at 389 deaths and 313 deaths respectively.
The number of deaths in 2016 for children and young people from respiratory diseases and infections has returned to similar levels observed in 2014, recovering from the small increases seen in the previous year.
Figure 11: Top 5 broad causes with the highest number of avoidable deaths in children and young people (aged 0 to 19 years)
UK, 2016
Source: Office for National Statistics, National Records of Scotland, Northern Ireland Statistics and Research Agency
Notes:
- Figures are for deaths registered in each calendar year.
- Deaths of non-residents are included in figures for the UK.
- See accompanying datasets for further details of the underlying causes of death included in the avoidable mortality definition.
Download this chart Figure 11: Top 5 broad causes with the highest number of avoidable deaths in children and young people (aged 0 to 19 years)
Image .csv .xls9. Concept of avoidable mortality
The concept of avoidable mortality was first introduced by Rutstein and others in the 1970s who argued that, in order to develop effective indicators of healthcare, lists of diseases which should not (or only infrequently) give rise to death or disability should be drawn up.
Rutstein also noted that the list of conditions considered to be avoidable would need to be updated in light of improvements in medical knowledge and practice, as well as social and environmental changes. Although avoidable mortality has been researched for the last three decades, there is little consensus among researchers about how to define it.
The list of causes of death used in defining avoidable mortality is primarily based on the cause lists produced by Nolte and McKee (2004) (PDF 852KB) and Page, Tobias and Glover (2006) (PDF 1MB).These cause lists were updated and amended to make them more relevant to the UK and to take account of more recent developments in healthcare public health policy. Changes to these lists were influenced by Wheller and others (2007), AMIEHS (2011) and views of respondents to the 2011 and 2015 consultations.
Statistics on avoidable mortality are used by central government, public health observatories, academia and charitable organisations working to reduce the prevalence of specific diseases and conditions deemed to be avoidable causes of death.
One of the main expected uses of these statistics is the monitoring of the quality performance of healthcare and public health policies. The Department of Health uses potential years of life lost (PYLL) from causes considered amenable to healthcare for children and the young in its NHS Outcomes Framework 2016 to 2017. It uses mortality from preventable causes as an indicator in its Public Health Outcomes Framework to reduce preventable ill-health, population dying prematurely and to reduce the gap between communities.
Further information on avoidable mortality indicators used at international level is available in the avoidable mortality quality and methodology information report.
Back to table of contents10. Quality and methodology
Age-standardised mortality rates were calculated using the number of potentially avoidable deaths registered in each year as the numerator and the mid-year population estimate for that year as the denominator.
Although age limits were set for some cause groups, rates were calculated using people of all ages as the denominator to allow data by cause group, amenable and preventable categories to be presented on a comparable basis. For the children and young people’s indicator, an upper age limit of 19 years was used to calculate age-standardised rates.
The avoidable mortality Quality and Methodology Information report contains important information on:
the strengths and limitations of the data and how it compares with related data
uses and users of the data
how the output was created
the quality of the output including the accuracy of the data
Office for National Statistics holds mortality data for England and Wales. Figures for the UK include data kindly provided by National Records of Scotland and the Northern Ireland Statistics and Research Agency.
Differences referred to in this bulletin are based on unrounded figures. A difference that is described as “statistically significant” has been assessed using 95% confidence intervals. If a difference is said to be statistically significant, it is unlikely that it could have occurred by chance alone. Confidence intervals give a measure of the statistical precision of an estimate and show the range of uncertainty around the estimated figure. As a general rule, if the confidence interval around an estimate overlaps with the interval around another, there is no significant difference between the two estimates. When the number of deaths is less than 100, the method used to calculate confidence intervals is different (see Dobson and others, 1991).
Back to table of contents
