Table of contents
- Main points
- Statistician’s comment
- Things you need to know about this release
- Upcoming changes to this bulletin
- UK alcohol-related deaths stable since 2012
- Comparisons between the 4 countries of the UK by sex, 1994 to 2015
- Regions of England
- How does the National Statistics definition differ from definitions developed by other government departments?
- Context and uses of these statistics
- Registration delays
- References
- Links to related statistics
- User-requested data
- Quality and methodology
1. Main points
In 2015, there were 8,758 alcohol-related deaths in the UK, an age-standardised rate of 14.2 deaths per 100,000 population.
For the UK as a whole, alcohol-related death rates have not changed in recent years, but the rate in 2015 is still higher than that observed in 1994.
The majority of alcohol-related deaths (65%) in the UK in 2015 were among males.
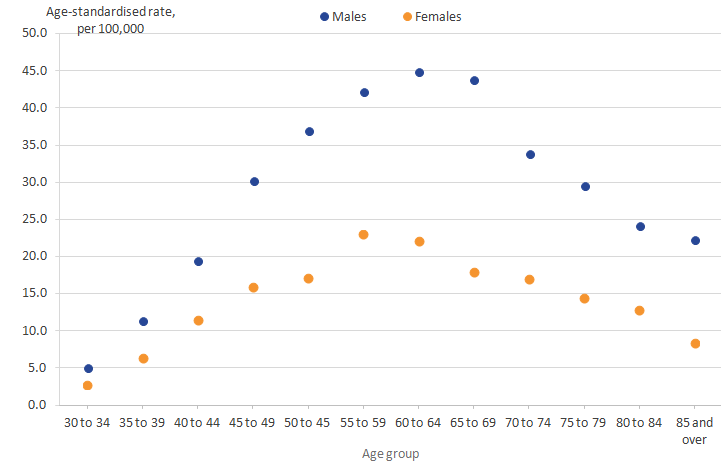
For both males and females, rates of alcohol-related death were highest in those aged 55 to 64 years in 2015.
Scotland remains the UK constituent country with the highest rate of alcohol-related deaths in 2015; yet, Scotland has also seen the largest decrease in its rates since they peaked in the early 2000s.
2. Statistician’s comment
“The statistics suggest that the prevalence of alcohol-related deaths has remained relatively stable over recent years. However, on a sub-UK level, it is notable that Scotland, the area with the highest numbers of alcohol-related deaths, has also seen the fastest reductions in mortality in recent years.”
Dr Annie Campbell, Health Analysis and Life Events, Office for National Statistics.
Back to table of contents3. Things you need to know about this release
What is the National Statistics definition of alcohol-related deaths?
The National Statistics definition of alcohol-related deaths includes underlying causes of death regarded as those being most directly due to alcohol consumption, as shown in Table 1. The definition is primarily based on chronic conditions associated with long-term abuse of alcohol and, to a lesser extent, acute conditions. Apart from poisoning with alcohol (accidental, intentional or undetermined), the definition excludes other external causes of death, such as road traffic and other accidents. The definition was developed for the purposes of monitoring alcohol-related deaths across all the constituent countries of the UK, using consistent methodology based solely on the information collected at death registration. Therefore, our definition differs from those developed within some constituent countries.
The definition does not include diseases that are partially attributable to alcohol, such as cancers of the mouth, oesophagus and liver. However, all deaths from chronic liver disease and cirrhosis (excluding biliary cirrhosis) are included, even when alcohol is not specifically mentioned on the death certificate.
Table 1: National Statistics definition of alcohol-related deaths, International Classification of Diseases, Tenth Revision (ICD-10)
| ICD-10 code | Description of Condition |
| F10 | Mental and behavioural disorders due to use of alcohol |
| G31.2 | Degeneration of nervous system due to alcohol |
| G62.1 | Alcoholic polyneuropathy |
| I42.6 | Alcoholic cardiomyopathy |
| K29.2 | Alcoholic gastritis |
| K70 | Alcoholic liver disease |
| K73 | Chronic hepatitis, not elsewhere classified |
| K74 | Fibrosis and cirrhosis of liver (Excluding K74.3-K74.5 - Biliary cirrhosis) |
| K86.0 | Alcohol induced chronic pancreatitis |
| X45 | Accidental poisoning by and exposure to alcohol |
| X65 | Intentional self-poisoning by and exposure to alcohol |
| Y15 | Poisoning by and exposure to alcohol, undetermined intent |
| Source: Office for National Statistics | |
Download this table Table 1: National Statistics definition of alcohol-related deaths, International Classification of Diseases, Tenth Revision (ICD-10)
.xls (27.1 kB)Figures are based on deaths registered in each calendar year, rather than occurring in each year. Since the majority of alcohol-related deaths registered in 2015 in England and Wales also occurred in that year (92%, 6,700 out of 7,298 deaths), registration delays are likely to have minimal impact on the findings. Further information about registration delays can be found in the section “Registration delays”.
Back to table of contents4. Upcoming changes to this bulletin
In the coming months we will be working to review our definition of alcohol-related deaths. This work is being conducted to improve the consistency of outputs on deaths related to the abuse of alcohol produced by different government departments across the UK. We will be holding a consultation on this definition in the summer of 2017 with the view to using an improved definition in our next release.
Back to table of contents6. Comparisons between the 4 countries of the UK by sex, 1994 to 2015
Since 1994, alcohol-related death rates in Scotland have tended to be higher for both sexes compared with the other constituent countries. Alcohol-related death rates amongst the other countries have, broadly speaking, been similar to each other over the period 1994 to 2015.
Most recently, all 4 UK constituent countries had higher rates of alcohol-related deaths in 2015 than in 1994 despite recent declining trends since the mid-2000s. These trends over time can be seen in Figures 3 and 4.
Males in Scotland experienced the fastest decrease in alcohol-related death rates since 2003
For males, since reaching a peak in the early 2000s, there has been a marked decrease in rates of alcohol-related deaths in Scotland. This decrease is greater than that for England, Wales or Northern Ireland, as shown in Figure 3. Despite the decrease in the alcohol-related death rate in Scotland among males, the rate in 2015 (30.0 per 100,000 males) remains higher than that in 1994 (23.3 per 100,000 males), when our time series began.
Northern Ireland data on alcohol-related deaths has a high degree of variability over time since 1994. In 2015, the alcohol-related death rate among males in Northern Ireland was 24.4 deaths per 100,000 males. Despite this rate being 20% higher than that observed in 2014, these 2 rates were not statistically different.
Alcohol-related death rates among males in England and Wales remain similar to those observed in recent years.
Figure 3: Age-standardised alcohol-related death rates per 100,000 males
UK constituent country, 1994 to 2015
Source: Office for National Statistics, National Records of Scotland, Northern Ireland Statistics and Research Agency
Notes:
- A common definition of alcohol-related death is used across the United Kingdom. See the ""Things you need to know"" section for more information.
- Rates are expressed per 100,000 population and standardised to the 2013 European Standard Population.
- Deaths of non-residents are included in figures for the UK.
- Figures are for deaths registered in each calendar year.
Download this chart Figure 3: Age-standardised alcohol-related death rates per 100,000 males
Image .csv .xlsAlcohol-related deaths among females are lowest in England
In 2015, the alcohol-related death rate among females in Northern Ireland was 12.4 deaths per 100,000 females. Despite the rate in 2015 being the highest for females in Northern Ireland since our records began in 1994, this rate was not statistically different to that observed in 2014. Since 1994, rates of alcohol-related deaths among females in Northern Ireland have been volatile, often fluctuating year-on-year. Despite the fluctuations, rates across time have often not been statistically different from each other as a result of the generally small number of deaths creating a wider degree of uncertainty around estimates.
As shown in Figure 4, there were minimal, statistically not significant changes in female alcohol-related death rates from 2014 to 2015 for the remaining UK constituent countries (England, Wales and Scotland). Across time, the lowest rates of alcohol-related deaths among females have typically been observed in England.
Figure 4: Age-standardised alcohol-related death rates per 100,000 females
UK constituent country, 1994 to 2015
Source: Office for National Statistics, National Records of Scotland, Northern Ireland Statistics and Research Agency
Notes:
- A common definition of alcohol-related death is used across the United Kingdom. See the ""Things you need to know"" section for more information.
- Rates are expressed per 100,000 population and standardised to the 2013 European Standard Population.
- Deaths of non-residents are included in figures for the UK.
- Figures are for deaths registered in each calendar year.
Download this chart Figure 4: Age-standardised alcohol-related death rates per 100,000 females
Image .csv .xls7. Regions of England
Alcohol-related death rates for both sexes remained highest in the North East in 2015
For both sexes, the North East had the highest alcohol-related death rate in 2015: for males this was 25.0 per 100,000 population and for females this was 14.4 per 100,000 population. The lowest alcohol-related death rate for males was 12.6 per 100,000 population observed in the East of England, consistent with previous years; for females, the lowest alcohol-related death rate was 6.1 per 100,000 females and occurred in London.
With the exception of London, alcohol-related death rates have increased in regions of England since the mid-1990s and have tended to be higher in the north of England relative to the south of England. Since the mid-2000s, the alcohol-related death rate has declined in London, which now has one of the lowest alcohol-related death rates, whereas the rate has remained comparatively high in the north of England. In recent years, there has been very little change in alcohol-related death rates and their pattern across the regions of England. This is shown in Figures 5 and 6 for males and females respectively.
Figure 5: Age-standardised rates of alcohol-related deaths for males, by region
England, 1995, 2005 and 2015
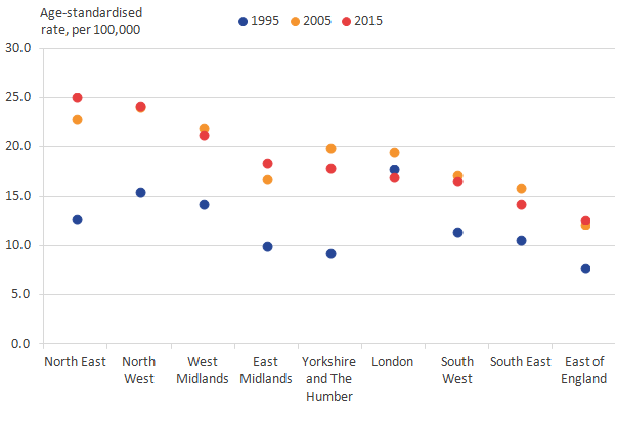
Source: Office For National Statistics
Notes:
- A common definition of alcohol-related death is used across the United Kingdom. See the "Things you need to know" section for more information
- Rates per 100,000 population, standardised to the 2013 European Standard Population
- Deaths of non-residents are excluded
- Figures are for deaths registered in 2015
- Regions are ordered from largest to smallest alcohol-related death rate in 2015
Download this image Figure 5: Age-standardised rates of alcohol-related deaths for males, by region
.png (16.0 kB) .xls (27.1 kB)
Figure 6: Age-standardised rates of alcohol-related deaths for females, by region
England, 1995, 2005 and 2015
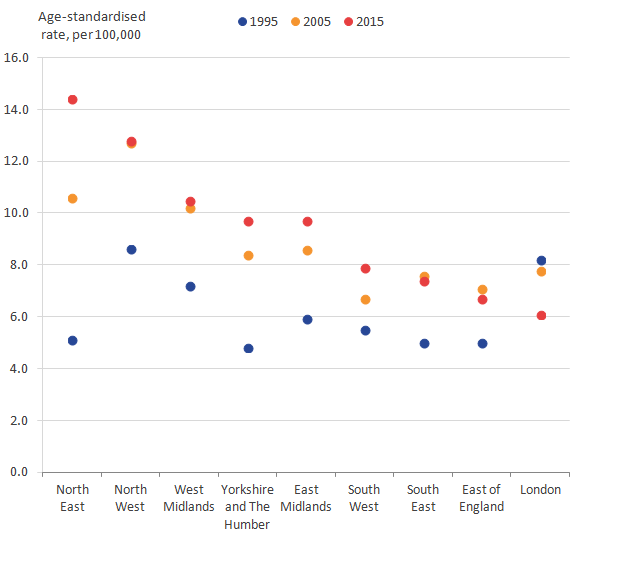
Source: Office For National Statistics
Notes:
- A common definition of alcohol-related death is used across the United Kingdom. See the "Things you need to know" section for more information
- Rates per 100,000 population, standardised to the 2013 European Standard Population
- Deaths of non-residents are excluded
- Figures are for deaths registered in 2015
- Regions are ordered from largest to smallest alcohol-related death rate in 2015
Download this image Figure 6: Age-standardised rates of alcohol-related deaths for females, by region
.png (11.9 kB) .xls (26.6 kB)A possible explanation for regional differences in alcohol-related deaths could be that those in deprived areas are differentially affected by the alcohol they consume. Specifically, the alcohol consumption harm paradox shows that consumption in more deprived areas can often be the same or even less than that in less deprived areas but harm is elevated in the more deprived areas. This could be due to the existence of other health problems, differences in drinking habits and access to healthcare (Jones et al, 2015). The geographic variation in alcohol-related death rates has been well documented in previous research. For example, Breakwell et al. (2007) reported a strong link between higher alcohol-related death rates and those living in the most deprived neighbourhoods of England and Wales. Similarly, Fone et al. (2013) showed that those living in the most deprived areas of Wales were more likely to demonstrate harmful binge drinking behaviour than those in the least deprived areas. Erskine et al. (2010) also supported these findings, additionally reporting higher risk of alcohol-related deaths in urban areas, after accounting for socio-economic status.
Back to table of contents8. How does the National Statistics definition differ from definitions developed by other government departments?
The National Statistics definition of alcohol-related deaths (see “Things you need to know”) was developed for the purposes of monitoring alcohol-related deaths across all the constituent countries of the UK, using consistent methodology based solely on the information collected at death registration. Therefore, our definition differs from those developed within some constituent countries. The section “Upcoming changes to this bulletin” describes how we will be working to harmonise these statistics.
Specifically, Public Health England (PHE), The Scottish Public Health Observatory (ScotPHO) and Public Health Wales (PHW) report alcohol deaths data using different definitions that aim to capture the wider burden of alcohol consumption on population health and health service use. A separate definition is not available for Northern Ireland, while PHW use the definition developed by PHE. These definitions include conditions where alcohol is the direct cause of all cases (also known as alcohol-specific or wholly-attributable conditions), as well as conditions where alcohol is causally implicated in some, but not all cases of the outcome (also known as partially-attributable conditions).
For partially-attributable conditions the proportion of cases that are caused by alcohol is calculated for each condition. For example, Jones and Bellis (2014) estimate that in England, 63% of oesophageal cancer cases among men and 51% among women aged 55 to 64 years are caused by alcohol consumption. In addition to chronic conditions like cancer and cardiovascular disease, some external causes of death such as road traffic accidents and falls are also attributable to alcohol. For example, Jones and Bellis (2014) estimate that among 35 to 44-year-olds in England, alcohol consumption is responsible for 37% of male and 20% female deaths due to falls.
The differences between our definition and those used by each public health organisation mentioned are similar, so we will only highlight the major ones using PHE as an example.
First, the term “alcohol-related” is used in different contexts by the Office for National Statistics (ONS) and PHE. As used by us, it refers to alcohol-specific or wholly-attributable conditions (for example, alcoholic liver disease), as well as all cases of certain liver diseases even when alcohol is not specifically mentioned on the death certificate. Conversely, as used by PHE, the term “alcohol-related” refers to wholly-attributable and partially-attributable conditions (for example, hypertensive diseases, various cancers and falls).
Second, we include all deaths from certain liver diseases – fibrosis and liver cirrhosis, and unspecified chronic hepatitis – in our definition on the assumption that, in England and Wales, many of them are caused by alcohol, even if this is not explicitly stated. Our assumption is based on the known under-reporting of alcoholism on death certificates due to death certifiers not being aware of previous alcoholism, or being uncertain of its relationship with the cause of death. It is our view that excluding deaths from these conditions will under-estimate the number of alcohol-related deaths. We exclude biliary cirrhosis, an autoimmune disease, from our definition because there is no evidence that it is associated with alcohol consumption. Conversely, PHE treat these liver diseases (including biliary cirrhosis) as partially-attributable to alcohol, so only a proportion of deaths from them are included in their alcohol-related deaths definition.
Third, although the list of wholly-attributable conditions in our definition and that of PHE is broadly similar, there are more of these alcohol-specific conditions on their list than on ours. One reason for this is that we only include the underlying cause of death in our definition, while PHE include conditions which are regarded as secondary causes, that is, those conditions that describe the nature of the injury sustained or other consequences of external causes of death.
There has been growing interest in the use of partially-attributable conditions to provide a truer burden of alcohol consumption on population health and use of health services associated with these conditions. For example, recent government guidelines recommend that both sexes consume no more than 14 units of alcohol per week and that these units should be spread over several days (Department of Health, 2016). These guidelines stem from evidence showing that more than 14 units of alcohol per week increases the risk of developing conditions that are partially attributable to alcohol (Holmes et al., 2016). Other government departments such as PHE use wholly and partially-attributable conditions to assess the wider impacts of alcohol consumption on hospital admissions (Public Health England, 2015).
The definitions of alcohol-related deaths developed by the public health organisations are not consistent and cannot be used to compare UK countries. We therefore recommend using the National Statistics definition to monitor trends for the UK and to make comparisons between its constituent countries. The country-specific definitions are useful in monitoring the wider impact of alcohol consumption within UK countries and for comparing local areas in England.
Back to table of contents9. Context and uses of these statistics
The harmful effects of alcohol on the human body can be categorised as acute (immediate) or chronic (longer-term). Examples of acute effects include reduced co-ordination and lowered inhibitions, while chronic effects include liver cirrhosis, heart disease and increased risk of developing liver, bowel and other forms of cancer (Cancer Research 2014). All types of alcoholic beverage (for example, beer, wine, spirits) increase the risk of certain cancers and recently it has been estimated that between 4 to 6% of new cancers in the UK are caused by alcohol consumption (COC, 2015).
In 2014, the UK consumed an average of 9.4 litres of alcohol per adult (defined as those aged 15 years and above; BBPA, 2015). Excessive drinking is estimated to result in approximately 3.3 million (5.9% of all deaths) deaths globally each year (WHO, 2014). This is greater than, for example, the proportion of deaths from HIV/AIDS (2.8%), violence (0.9%) or tuberculosis (1.7%) (WHO, 2014). In England, alcohol misuse costs the National Health Service (NHS) around £3.5 billion per year (House of Commons Health Committee, 2012).
Given the harmful effects of excessive alcohol consumption, there is widespread policy, professional and public interest in the prevalence of alcohol-related deaths in the UK. The main users of these statistics include the Department of Health and devolved government administrations, public health organisations and local government. The figures on alcohol-related deaths are used to monitor and develop policies to protect the health of the general public.
Most recently Public Health England published an evidence review of the public burden of alcohol and the effectiveness and cost-effectiveness of alcohol control policies (Public Health England, 2016). In this report ONS data on alcohol-related deaths are used extensively to report the impact alcohol has on deaths of working age individuals.
In January 2016, the government published new guidelines for alcohol consumption (Department of Health, 2016), recommending that men and women should drink no more than 14 units of alcohol per week and that these units should be spread across several days. These new guidelines outline the government’s commitment to protecting the population from serious health threats, helping people to live longer, healthier and more fulfilling lives. The Home Office’s Alcohol Strategy (2012) initiated a consultation on banning multi-buy alcohol discounting in order to reduce the number of people drinking to harmful levels.
Non-government users of these statistics include non-profit organisations such as Drinkaware and Addaction. These organisations use the statistics to raise awareness of the potential risks associated with excessive drinking habits, to target support services to groups at risk of experiencing adverse consequences of alcohol consumption and to inform public opinion and government policy. Many of these organisations have signed up as partners to the government’s Public Health Responsibility Deal (Department of Health, 2014). Academics and researchers also use the statistics to investigate the cause and impacts of alcohol-related deaths.
These statistics are of interest to the general public. Local and national media report on alcohol-related death trends and geographical patterns and may comment on the effectiveness of current or proposed government policies.
This statistical bulletin presents figures for the UK, England and Wales, and English regions. Statistics for Scotland are also published by the National Records of Scotland while those for Northern Ireland are published by the Northern Ireland Statistics and Research Agency.
Back to table of contents10. Registration delays
The information used to produce mortality statistics is based on the details collected when deaths are certified and registered. In England and Wales, deaths should be registered within 5 days of the death occurring, but there are some situations that result in the registration of the death being delayed. Deaths considered unexpected, accidental or suspicious will be referred to a coroner who may order a post mortem or carry out a full inquest to ascertain the reasons for the death.
In 2015, the average (median) time taken for a death to be registered in England and Wales was 6 days. The majority of alcohol-related deaths registered in 2015 also occurred in that year (92%). The average registration period for alcohol-related deaths in Scotland and Northern Ireland were 3 days and 6 days respectively.
Back to table of contents11. References
British Beer and Pub Association (BBPA) (2015). Alcohol Consumption Data. [Accessed 20/01/2017]
Breakwell C, Baker A, Griffiths C, Jackson G, Fegan G and Marshall D (2007). Trends and geographical variations in alcohol-related deaths in the United Kingdom, 1991-2004. Health Statistics Quarterly 33, 6-22. [Accessed 20/01/2017]
Cancer Research (2014). Alcohol and Cancer. [Accessed 18/1/2017]
Committee on Carcinogenicity of Chemicals in Food, Consumer Products and the Environment (COC) (2015) Statement on the consumption of alcoholic beverages and risk of cancer. [Accessed 13/01/2017]
Department of Health (2016). UK Chief Medical Officers’ Alcohol Guidelines Review: summary of the proposed new guidelines. [Accessed 20/01/2017]
Department of Health (2014). Public Health Responsibility Deal. [Accessed 20/01/2017]
Erskine S, Maheswaran R, Pearson T and Gleeson D (2010). Socioeconomic deprivation, urban-rural location and alcohol-related mortality in England and Wales. BMC Public Health, 10:99. [Accessed 18/01/2017]
Fone D, Farewell D, White J, Lyons R and Dunstan F (2013). Socioeconomic patterning of excess alcohol consumption and binge drinking: a cross-sectional study of multilevel associations with neighbourhood deprivation. British Medical Journal, 3:4. [Accessed 17/12/2017]
Holmes J, Angus C, Buykx P, Ally A, Stone T, Meier P and Brennan A (2016). Mortality and morbidity risks from alcohol consumption in the UK: Analyses using the Sheffield Alcohol Policy Model (v,2.7) to inform the UK Chief Medical Officers’ review of the UK lower risk drinking guidelines. [Accessed 18/01/2017]
Home Office (2012). Alcohol Strategy. [Accessed 20/01/2017]
House of Commons Health Committee (2012). Government’s Alcohol Strategy [Accessed 18/01/2017]
Jones L and Bellis M (2014). Updating England-Specific Alcohol-Attributable Fractions. [Accessed 17/01/2017]
Jones L Bates J McCoy E and Bellis M (2015). Relationship between alcohol-attributable disease and socioeconomic status, and the role of alcohol consumption in this relationship: a systematic review and meta-analysis. BMC Public Health 15, 400 [Accessed 31/01/2017]
Office for National Statistics (2016) ‘Adult Drinking Habits in Great Britain: 2014’ [Accessed 17/01/2017]
Public Health England (2006). Alcohol consumption in adults [Accessed 17/01/2017]
Public Health England (2016). ‘The Public Health Burden of Alcohol and the Effectiveness and Cost-effectiveness of Alcohol Control Policies: An evidence review’ [Accessed on 17/01/2017]
World Health Organisation (2014). Global Status Report on Alcohol and Health 2014. [Accessed 18/01/2017]
Back to table of contents13. User-requested data
Special extracts and tabulations of alcohol-related death (and other causes of mortality) data for England and Wales are available to order for a charge (subject to legal frameworks, disclosure control, resources and agreement of costs, where appropriate). Such requests or enquiries should be made to:
Mortality Analysis Team, Life Events and Population Sources Division
Office for National Statistics
Government Buildings
Cardiff Road
Newport
South Wales
NP10 8XG
Tel: +44 (0)1633 456736
Email: mortality@ons.gov.uk
Our charging policy is available on our website.
Back to table of contents14. Quality and methodology
The Alcohol-related deaths Quality and Methodology Information document contains important information on:
the strengths and limitations of the data and how it compares with related data
uses and users of the data
how the output was created
the quality of the output including the accuracy of the data
Statistics on mortality are derived from the information provided when deaths are certified and registered. Further information about the methods and quality of these statistics can be found in the Quality and Methodology document. ONS holds mortality data for England and Wales. Figures for the UK include data kindly provided by National Records of Scotland and the Northern Ireland Statistics and Research Agency.
Differences referred to in this bulletin are based on unrounded figures. A difference which is described as “statistically significant” has been assessed using 95% confidence intervals. If a difference is said to be statistically significant, it is unlikely that it could have occurred by chance alone. Confidence intervals give a measure of the statistical precision of an estimate and show the range of uncertainty around the estimated figure. As a general rule, if the confidence interval around an estimate overlaps with the interval around another, there is no significant difference between the 2 estimates. When the number of deaths is less than 100, the method used to calculate confidence intervals is different (see Dobson et al., 1991).