1. Statistician’s Comment
“In the 1950s there was very little difference between life expectancy and the ages at which people finished working – particularly for men. Now, on average, men can expect to live around 15 years and women can expect to live around 20 years after they stop working. Living longer means that the population aged 65 years and over is growing faster than the working age population aged 16 to 64 years.
“Within the older working age population, there are 866,000 potential workers aged 50 to 64 years who would like to work but can’t. Ill-health is the main barrier preventing just over a third from working. Additionally, half of people in this age group have at least one living parent and just under half have a grandchild, so caring for others is likely to be a barrier for some.
“Workers aged in their 50s and early 60s are more likely than any other age group to be juggling caring responsibilities and working. In 2016 to 2017, 65% of men and 60% of women aged 52 to 64 years who were carers were also in work.”
Sarah Crofts, ONS Centre for Ageing and Demography
Back to table of contents2. Why is it important that people extend their working lives?
In 1960, there was very little difference between life expectancy and the age at which a person left the workforce – particularly for men. Now men can expect to live for around 15 years and women around 20 years after leaving the workforce. This means on average people in the UK are spending longer in retirement. This can have benefits for individuals including the opportunity to contribute more to society through voluntary work and other community activities and to enjoy a longer retirement.
Living longer does present the government and society with some challenges. Our older population is growing more rapidly than the population of working age. At the same time, the age at which people leave the labour force has not kept pace with increases seen in average life expectancy (Figure 1).
Figure 1: Average age of exit from work has not been keeping pace with increases in life expectancy
Difference between life expectancy and average age of exit from the labour force, men and women, 1960 to 2018, UK
Source: Department for Work and Pensions – Economic and labour market status of individuals aged 50 and over, trends over time: October 2018 (experimental), Office for National Statistics
Download this chart Figure 1: Average age of exit from work has not been keeping pace with increases in life expectancy
Image .csv .xlsGiven the ageing workforce and scale of early exit from the labour market, the future UK economy is likely to face significant challenges in areas such as the financing of State Pension provision and maintaining the supply of labour. Individuals may also need to consider working until later in life to ensure adequate retirement income.
Extending working lives can also bring many positive benefits to individuals. Financial stability and better health and well-being are some of these benefits. However, these are dependent on the “quality of work” – for example, whether work is flexible to enable older workers to meet other demands on their time and whether the employee has a level of choice over the work they do (A silver lining for the UK economy?).
The government’s Industrial Strategy aims to address potential skills gaps and age bias in the work place. It is estimated if the employment rate of people aged 50 to 64 matched that of those aged 35 to 49, it would add more than 5% to UK GDP, or £88 billion.
Increasing numbers of people are working at older ages, but there are people below state pension age who would like to work but can’t. Men aged 50 to 64 years are more likely to be in employment than women of these ages1. People who want to work in this age group are often referred to as the ‘missing million’, although latest figures estimate the number to be just under this at 866,0002.
Figure 2: Over a third of people aged 50 to 64 years who would like to work, are out of work because they are sick or disabled
Reasons for being out of work for those aged 50 to 64 years who would like to work, men and women, 2018, UK
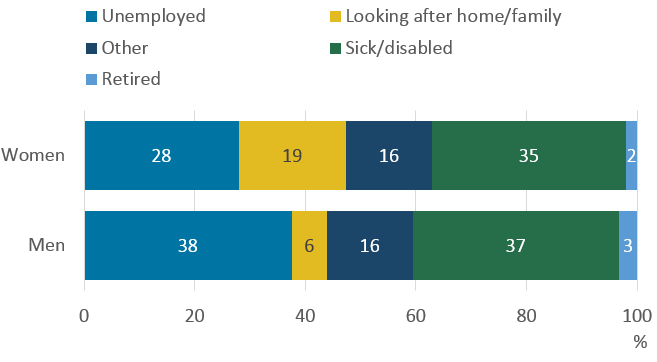
Source: Office for National Statistics – Annual Population Survey
Download this image Figure 2: Over a third of people aged 50 to 64 years who would like to work, are out of work because they are sick or disabled
.png (13.6 kB) .xls (53.2 kB)Of those potential older workers who are out of work (but would like to work), 38% of men and 28% of women are unemployed. Women are more likely to be looking after home or family than men (19% and 6%). Ill health is the main barrier to working for both men (37%) and women (35%).
Back to table of contents3. How does health affect employment?
The better a person’s health the more likely it is they will be working2. 44% of those aged 50 to 64 years have a health problem lasting or expecting to last more than a year. Over half of these people (58%) were working in the previous month, compared to 81% of people without a health problem2.
Figure 3: People aged 50 to 64 years with a long-term health problem are less likely to be working
Employment status by long-term health problem, 2017 to 2018, UK
Source: Office for National Statistics – Annual Population Survey
Download this chart Figure 3: People aged 50 to 64 years with a long-term health problem are less likely to be working
Image .csv .xls13% of men and 45% of women aged 50 to 64, worked part-time in 2017 to 20182. Having a health problem makes little difference to this pattern. Both male and female workers with health problems are more likely to work part-time than workers without health problems, but the differences are small.
People aged 50 to 64 years with certain health conditions are less likely to be in work than those with other health conditions. Over 80% of those with learning difficulties and certain mental health issues are not in paid work. Many of those with health problems do work, including around half of those with depression and over 60% of those with skin conditions or allergies, difficulty in hearing, diabetes, heart and circulatory issues, breathing problems and stomach and digestion problems2.
Back to table of contents4. How does caring affect employment?
"A carer is considered to be anyone who spends time looking after or helping a friend, family member or neighbour who, because of their health and care needs, would find it difficult to cope without this help regardless of age or whether they identify as a carer."
Carers Action Plan 2018 - 2020 Supporting carers today, Department of Health and Social Care
In 2016 to 2017, of all people aged 52 to 64 years, 50% still had at least one living parent, 82% had at least one child, and 45% had a grandchild. Additionally, 75% of men and 65% of women aged 52 to 64 were working3 People in this age group are more likely than any other age group to be carers4 and many will be working at the same time. One in four women and around one in seven men provided care for someone in the last week in 2016 to 20173.
In 2016 to 2017, 65% of men and 60% of women aged 52 to 64 years who were caring were also in work.
Figure 4: People aged 52 to 64 years who are carers are less likely to be in employment than those who are not carers
Men and women aged 52 to 64 years in employment by caring status, 2016 to 2017, England
Source: NatCen Social Research, University College London and Institute for Fiscal Studies – English Longitudinal Study of Ageing
Notes:
- Age range defined as 52 to 64 years because by 2016 to 2017 the 50-year-olds from the last sample refresh in the English Longitudinal Study of ageing have aged and not been replaced.
Download this chart Figure 4: People aged 52 to 64 years who are carers are less likely to be in employment than those who are not carers
Image .csv .xlsWorkers over the age of 50 years are most likely to say that working part-time and flexible working hours would help them delay retirement5, this is particularly important for those managing health conditions and/or caring responsibilities.
Comparing men and women aged 52 to 64 years who both work and care, women are far more likely to work part time. Among women who both care and work, 65% are part-time workers compared with 18% of men3.
Figure 5: Men aged 52 to 64 years who care for someone whilst working are as likely to work full-time as those who aren’t caring for anyone
Percentage working part time by caring status for people aged 52 to 64 years, England
Source: NatCen Social Research, University College London and Institute for Fiscal Studies – English Longitudinal Study of Ageing
Download this chart Figure 5: Men aged 52 to 64 years who care for someone whilst working are as likely to work full-time as those who aren’t caring for anyone
Image .csv .xls5. Fitting it all in
We have looked at two important barriers to working for those in their 50s and early- to mid-60s – health and caring.
Although people in their 50s and early 60s have a good level of general health the prevalence of health problems increases over this age range and impacts on the likelihood of being in paid work. People with learning difficulties or certain mental health issues are less likely to work than those with depression or physical health problems. Latest health life expectancy (HLE) figures show that for both men and women, HLE in the most deprived areas of the UK and for the most disadvantaged social groups is well below state Pension age. The government’s industrial strategy includes the mission to increase healthy independent expectancy by five years by 2035, while narrowing the gap between the experience of the richest and poorest.
Women in particular are trying to “fit it all in”. Our analysis has shown that a higher percentage of women aged 52 to 64 years provide care than men while at the same time the percentage of women in their 50s and 60s who work has been rising over recent decades and is now higher than ever before.
Care giving for women aged 45 to 64 years can be associated with increased social activity6 (this includes caring for dependent children). However, for the most-part, informal care giving can be a mentally and physically demanding responsibility, which can negatively affect a person’s overall health7,8 and in turn, their ability to work. Research has shown those who combine work and care often do so at personal cost such as tiredness, ill-health and lack of leisure.
A recent study showed few employees want to give up work in order to take on caring responsibilities. However, decisions about working were based on a combination of factors, including financial considerations, health, job satisfaction and stress, as well as caring responsibilities. Flexible working hours and part time options are most likely to encourage people in their 50s to continue working for longer5.
A more detailed report on older workers will be published in early 2019. Future articles in the living longer series will include the implications of an ageing population for households and housing, economy and finance, health well-being and staying connected.
Back to table of contents6. References
Office for National Statistics, Labour Force Survey
Office for National Statistics, Annual Population Survey
NatCen Social Research, University College London and Institute for Fiscal Studies, English Longitudinal Study of Ageing
NatCen, British Social Attitudes Survey, 2015
Evandrou, M and Glaser, K, (2015) "Economic and Social Roles in Midlife in Britain" in Aging and Caring at the Intersection of Work and Home Life: Blurring the Boundaries. Edited by Martin-Matthews, A and Philips, J. E., p207 to 228.
Pinquart & Sörensen (2007) "Differences between caregivers and noncaregivers in psychological health and physical health: a meta-analysis" Psychology and Ageing 18(2):250 to 67
Lacey, R E, McMunn, A and Webb, E 2018 Informal caregiving patterns and trajectories of psychological distress in the UK Household Longitudinal Study. Journal of Psychological Medicine
