Table of contents
- Main points
- Things you need to know about this release
- How have we defined avoidable mortality?
- Males were more likely to die from an avoidable cause than females
- There were significant increases in the avoidable mortality rate for respiratory diseases and injuries
- Cardiovascular disease accounted for 43% of all deaths from conditions deemed amenable to healthcare
- Neoplasms caused 39% of all deaths from preventable conditions
- Ischaemic heart disease accounted for 16% of all avoidable deaths in 2015
- Avoidable mortality rates increased in Wales in 2015 but remained stable in England
- Deaths from respiratory diseases considered avoidable increased in Wales in 2015
- The North East and North West of England had highest avoidable mortality rates in 2015
- Males accounted for almost two-thirds of avoidable deaths in children and young people
- Suicide and self-inflicted injuries caused most avoidable deaths in children and young people
- Avoidable deaths resulted in an average loss of 23 years of life
- What has changed in this release?
- Concept of avoidable mortality
- References
- Upcoming changes to this bulletin
- Data requests
- Quality and methodology
1. Main points
In 2015, approximately 23% of all deaths were from causes considered avoidable (119,485 deaths out of 529,655 deaths).
There were significant overall increases in the avoidable mortality rate for respiratory diseases and injuries, driven by an increase in Wales.
Deaths from neoplasms were the leading cause of avoidable deaths accounting for over a third (35%) of all avoidable deaths in 2015.
Males accounted for almost two-thirds (63%) of avoidable deaths in children and young people.
The highest number of avoidable deaths in children and young people were from suicide and self-inflicted injuries, which increased by 13% since 2014.
2. Things you need to know about this release
Figures in this release are presented for causes of death that are considered avoidable in the presence of timely and effective healthcare or public health interventions (avoidable mortality).
While a particular condition can be considered avoidable, this doesn’t mean that every death from that condition could be prevented. This is because factors such as the lifestyle and age of the patient, the extent of disease progression at diagnosis and the potential existence of other medical conditions are not taken into account when making a list of causes.
For most of the causes of death included in our definition there is an upper age limit of 74 years. This is because deaths at older ages are often difficult to attribute definitively to a single underlying cause and the chances of death are more affected by coexisting medical conditions and other factors.
It is widely accepted that the contribution of healthcare to improvements in population health ought to be quantified. Avoidable mortality, which is based on the concept that premature deaths from certain conditions should be rare and ideally should not occur in the presence of timely and effective healthcare, is used as an indicator to measure this contribution.
Avoidable mortality was not intended to serve as a definitive source of evidence of differences in effectiveness of healthcare systems. It was designed to highlight areas of potential weakness in healthcare that could benefit from further in-depth investigation. Therefore, a degree of caution is recommended when interpreting the data. Further information about the limitations of the concept of avoidable mortality is available in the avoidable mortality quality and methodology information notes.
With advances in medical technology and wider public health interventions, deaths from a condition that was previously not avoidable may have since become avoidable. This means that when the list of avoidable causes of death is updated, it may not be appropriate to produce previously published data using the revised avoidable mortality definition. For this reason, data presented in this bulletin are from 2014 onwards – the data year in which we implemented the revised definition. Where comparisons with the most recent available data for 2015 are discussed in the bulletin, these should not be interpreted as long-term trends. When differences are identified as statistically significant they can be interpreted as meaningful; otherwise they may simply have occurred because of year-on-year fluctuation.
Back to table of contents3. How have we defined avoidable mortality?
Amenable mortality:
- a death is amenable (treatable) if, in the light of medical knowledge and technology available at the time of death, all or most deaths from that cause (subject to age limits if appropriate) could be avoided through good quality healthcare
Preventable mortality:
- a death is preventable if, in the light of understanding of the determinants of health at the time of death, all or most deaths from that cause (subject to age limits if appropriate) could be avoided by public health interventions in the broadest sense
Avoidable mortality:
- avoidable deaths are all those defined as preventable, amenable (treatable) or both, where each death is counted only once; where a cause of death is both preventable and amenable, all deaths from that cause are counted in both categories when they are presented separately
4. Males were more likely to die from an avoidable cause than females
In 2015, approximately 23% of all deaths were from causes considered avoidable (119,485 deaths out of 529,655 deaths). The age-standardised avoidable mortality rate for all persons in England and Wales increased slightly to 223 per 100,000 population in 2015, however, this was not a significant increase when compared with 2014 data.
Figure 1: Number of deaths considered avoidable as a proportion of all deaths registered in 2015
England and Wales, 2015
Source: Office for National Statistics
Notes:
Figures are for deaths registered in the calendar year 2015.
Figures include deaths of non-residents.
Download this chart Figure 1: Number of deaths considered avoidable as a proportion of all deaths registered in 2015
Image .csv .xlsOf the avoidable deaths in 2015, males accounted for 60%: the same as found in 2014. In 2015, we found that approximately 28% of all male deaths were from avoidable causes (71,670 out of 257,207 deaths). On the other hand, around 18% of all female deaths were from avoidable causes (47,815 out of 272,488 deaths). The differences between males and females could be explained by gender protective factors. For example, research has found that hormones such as oestrogen can protect premenopausal women against heart disease (Nadkarni et al., 2011).
As a result, the rate for males was significantly higher at 278 deaths per 100,000 compared with 171 per 100,000 for females.
Back to table of contents5. There were significant increases in the avoidable mortality rate for respiratory diseases and injuries
There were significant increases in the avoidable mortality rate for respiratory diseases and injuries from 2014 to 2015 (11% and 5% respectively). The increase could partly be due to the increase in deaths from chronic lower respiratory diseases (which includes ICD10 codes J40 to J47) – one of the top five leading causes of deaths for males and females as found in Deaths registered in England and Wales in 2015 (Death Registrations, ONS, 2016a).
Injuries as a broad cause include those that were intentional (for example, suicide and self-inflicted injuries) and those that were unintentional (for example, transport accidents). Further analysis undertaken on injuries found that overall for both males and females in England and Wales there was an increase in both intentional and unintentional injuries. However, there was a larger increase in intentional injuries compared with unintentional injuries between 2014 and 2015.
The leading cause of avoidable deaths for broad cause groups was neoplasms (cancers and other non-cancerous tissue growths) for a second year in England and Wales. There was a decline in the age-standardised mortality rate for neoplasms in England and Wales, from 78 deaths per 100,000 population to 77 per 100,000; however, this decline was not statistically significant.
In contrast, the cause group with the lowest avoidable mortality rate was infections at 3.2 deaths per 100,000 population, which has slightly increased from 3.0 deaths per 100,000 as found in 2014.
For all other broad cause groups, the age-standardised avoidable mortality rate remained at similar levels in 2015 compared with 2014.
Figure 2: Avoidable mortality rates by broad cause group
England and Wales, 2014 to 2015
Source: Office for National Statistics
Notes:
Figures are for deaths registered in each calendar year.
Figures include deaths of non-residents.
Age-standardised rates per 100,000 population, standardised to the 2013 European Standard Population. Age-standardised rates are used to allow comparison between populations which may contain different proportions of people of different ages.
See dataset 1 for further details of the underlying causes of death included.
The 'Other' cause group consists of nutritional, endocrine and metabolic disorders, neurological disorders, digesitve disorders, genitourinary disorders, and maternal and infant conditions.
Download this chart Figure 2: Avoidable mortality rates by broad cause group
Image .csv .xls6. Cardiovascular disease accounted for 43% of all deaths from conditions deemed amenable to healthcare
There were 64,277 deaths from causes considered amenable to healthcare in England and Wales in 2015, an age-standardised rate of 121 deaths per 100,000 population.
Cardiovascular disease accounted for 43% of these deaths in England and Wales; 27,806 out of 64,227 deaths from amenable causes.
On the whole, there was very little change in the amenable mortality rate across all broad groups between 2014 and 2015. The largest change was in respiratory diseases, which increased from 24 deaths per 100,000 population to 26 deaths as a result of 1,374 more deaths in 2015.
Back to table of contents7. Neoplasms caused 39% of all deaths from preventable conditions
There were 99,725 deaths from causes that were considered preventable in light of wider public health interventions in England and Wales in 2015; an age-standardised rate of 186 deaths per 100,000 population.
Neoplasms (cancers and other non-cancerous tissue growths), were the leading cause of preventable deaths, accounting for 39% of deaths from conditions considered preventable, a slight decline compared with 2014.
Overall, there was little change in the preventable mortality rate across all broad groups between 2014 and 2015. The largest change in rate was found in injuries where the rate increased from 36 deaths per 100,000 population to 37 deaths per 100,000 as a result of 953 more deaths in 2015.
Back to table of contents8. Ischaemic heart disease accounted for 16% of all avoidable deaths in 2015
The broad cause categories of avoidable mortality can be further subdivided into specific causes of death (numbers of deaths by 5-year age group can be found in dataset 2). Ischaemic heart disease (IHD) is the specific cause with the highest number of avoidable deaths accounting for 16% of all avoidable deaths in 2015 (19,602 out of 119,485 avoidable deaths).
Ischaemic heart disease was also one of the leading causes of all deaths in England and Wales in 2015 (ONS, 2016a). Given the high number of avoidable deaths from IHD, it becomes difficult to assess the contribution of other causes of death to avoidable mortality. It is likely that any change in avoidable mortality figures will be heavily influenced by changes in the number of deaths from IHD. For this reason, we exclude IHD from the figures for avoidable mortality in this section.
Removing IHD from the avoidable mortality definition reduced the total number of avoidable deaths for persons in England and Wales to 99,883 deaths. This is an age-standardised rate of 186 deaths per 100,000 population and is significantly lower than the age-standardised avoidable mortality rate when IHD is included (a 17% decrease from 223 deaths per 100,000 population). A similar percentage decrease was observed in England and Wales separately.
The impact of removing IHD was greater for amenable mortality than preventable mortality. For amenable mortality there was a 31% decrease in age-standardised rate from 121 deaths per 100,000 population to 84 deaths per 100,000 population. For preventable mortality, the age-standardised rate decreased by 20% from 186 deaths per 100,000 population to 149.1 deaths per 100,000 when IHD was removed.
Excluding IHD resulted in a greater percentage decrease in rates for males than for females. In England and Wales (combined), rates for males fell by 21%, from 278 per 100,000 to 211 per 100,000, while those for females fell by 10% from 171 to 153.5 per 100,000. A similar picture was observed in both countries separately.
Figure 3: Age-standardised avoidable, amenable and preventable mortality rates with and without deaths from ischaemic heart disease (IHD)
England and Wales, 2015
Source: Office for National Statistics
Notes:
Figures are for deaths registered in the calendar year 2015.
Figures include deaths of non-residents.
Age-standardised rates per 100,000 population, standardised to the 2013 European Standard Population. Age-standardised rates are used to allow comparison between populations which may contain different proportions of people of different ages.
See dataset 1 for further details of the underlying causes of death included.
Download this chart Figure 3: Age-standardised avoidable, amenable and preventable mortality rates with and without deaths from ischaemic heart disease (IHD)
Image .csv .xls9. Avoidable mortality rates increased in Wales in 2015 but remained stable in England
Overall, avoidable mortality rates were significantly higher for persons in Wales compared with persons in England in 2015 (256 deaths per 100,000 population in Wales, 220 deaths per 100,000 population in England). Additionally, Wales saw a significant increase in avoidable mortality rates from 2014 to 2015, an increase from 240 per 100,000 population to 256 per 100,000 population; whereas age-standardised rates of avoidable mortality remained stable in England.
The breakdown of avoidable mortality rates by broad cause group shows that the increase in rate in Wales was driven by increases in the mortality rates for respiratory diseases and for injuries. The mortality rate for respiratory disease in Wales increased by 29% from 25 deaths per 100,000 population in 2014 to 32 deaths per 100,000 in 2015. For injuries, there was an increase in the avoidable mortality rate of 19% from 37 per 100,000 population in 2014 to 44 per 100,000 in 2015. The rates for these cause groups also increased from 2014 to 2015 in England but not to the same extent as they did in Wales; the rate for respiratory disease increased by 7% and the rate for injuries increased by 3%.
Back to table of contents10. Deaths from respiratory diseases considered avoidable increased in Wales in 2015
Similar patterns were observed for amenable and preventable mortality in England and Wales separately, where there was an increase in mortality rates in Wales for both amenable and preventable mortality from 2014 to 2015. The increase in amenable mortality for Wales was influenced by the significant increase in respiratory diseases amenable to healthcare. Meanwhile, the increase in preventable mortality rate in Wales was affected by significant increases in preventable mortality rates in a range of conditions including cardiovascular diseases and respiratory diseases from 2014 to 2015. There was no significant change in either the amenable mortality rate or preventable mortality rate in England between 2014 and 2015.
Figure 4: Age-standardised avoidable mortality rates by sex
England and Wales separately, 2014 to 2015
Source: Office for National Statistics
Notes:
Figures are for deaths registered in each calendar year.
Figures exclude deaths of non-residents.
Age-standardised rates per 100,000 population, standardised to the 2013 European Standard Population. Age-standardised rates are used to allow comparison between populations which may contain different proportions of people of different ages.
See dataset 1 for further details of the underlying causes of death included.
Download this chart Figure 4: Age-standardised avoidable mortality rates by sex
Image .csv .xls11. The North East and North West of England had highest avoidable mortality rates in 2015
The region with the highest avoidable mortality rate for males was the North East with a rate of 329 deaths per 100,000 males and for females it was the North West with a rate of 213 deaths per 100,000 females. These rates were also significantly higher than the England and Wales average.
Conversely, the region with the lowest rates was the South East for both males (236 per 100,000) and females (145 per 100,000). These rates were also significantly lower than the England and Wales average.
Rates were significantly higher for males than females in all English regions.
Figure 5: Age-standardised avoidable mortality rates for all persons
English regions and Wales, 2015
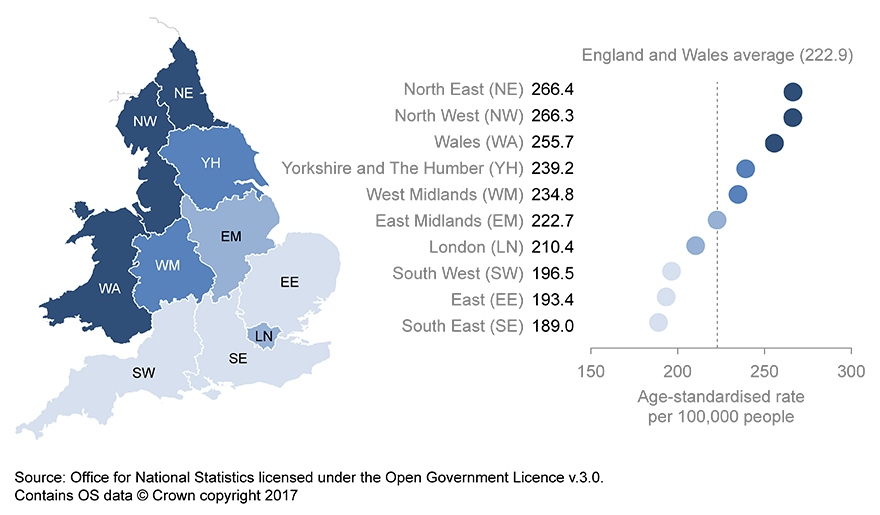
Source: Source: Office for National Statistics licensed under the Open Government Licence v.3.0. Contains OS data © Crown Copyright 2017
Notes:
Figures exclude those not usually resident in the areas shown.
See dataset 1 for a definition of avoidable mortality.
Download this image Figure 5: Age-standardised avoidable mortality rates for all persons
.png (144.6 kB) .xls (27.6 kB)12. Males accounted for almost two-thirds of avoidable deaths in children and young people
In 2015, of all deaths in children and young people aged 0 to 19 years in England and Wales, 31% (or 1,440 out of 4,582) were from causes considered avoidable through good quality healthcare and wider public health interventions. This was a very small decrease compared with 2014 and overall, avoidable deaths in children and young people made up 1% of the total number of avoidable deaths in 2015.
In England and Wales, males aged 0 to 19 accounted for almost two-thirds (63% or 896 out of 1,440 deaths) of avoidable deaths in children and young people. The rate for males was significantly higher than that for females at 13 deaths per 100,000 population compared with 8 per 100,000 respectively.
A similar pattern was observed in England and Wales separately where there was a higher avoidable mortality rate in males aged 0 to 19 compared with females. In England, the rates for males were significantly higher at 12 deaths per 100,000 population compared with 8 per 100,000 for females. There was no significant difference between males and females in Wales. Overall, the rate for males in Wales was higher compared with males in England but the reverse was observed for females.
Back to table of contents13. Suicide and self-inflicted injuries caused most avoidable deaths in children and young people
The single cause with the highest number of avoidable deaths in children and young people was suicide and self-inflicted injuries (14% or 206 deaths of all avoidable deaths in this age group).
Of the top five causes of avoidable deaths among children and young people, suicide and self- inflicted injuries was the only cause to see an increase since 2014 by 13% or 24 deaths. The other top causes each saw a decline since 2014, with accidental injuries, which was the leading cause in 2014, experiencing the largest decline of 8% or 15 deaths.
In comparison with the leading causes of avoidable deaths for those aged 0 to 74, avoidable deaths in children and young people tended to be as a result of non-chronic conditions such as injuries and accidents whereas for older people it was neoplasms and cardiovascular disease.
Figure 6: Top 5 causes with the highest number of avoidable deaths in children and young people (aged 0 to 19 years)
England and Wales, 2014 to 2015
Source: Office for National Statistics
Notes:
Figures are for deaths registered in each calendar year.
Figures for England and Wales include deaths of non-residents.
See dataset 3 for the definition of avoidable mortality in children and young people.
Download this chart Figure 6: Top 5 causes with the highest number of avoidable deaths in children and young people (aged 0 to 19 years)
Image .csv .xls14. Avoidable deaths resulted in an average loss of 23 years of life
In addition to reporting age-standardised rates of avoidable mortality, we have also calculated avoidable mortality using standardised years of life lost (SYLL). This indicator is a measure of the potential number of years lost when a person dies prematurely from any cause. The method weights deaths from those at younger ages more heavily than those at older ages.
In England and Wales in 2015, there were 5,999 years of life lost per 100,000 males who died from an avoidable cause, compared with 3,972 years of life lost per 100,000 females. These figures are similar to those reported for 2014. To put these figures into context, on average, each person who died from an avoidable cause lost 23 potential years of life; this has not changed between 2014 and 2015.
In children and young people, 878.4 potential years of life were lost per 100,000 males due to death from avoidable causes. For females there were 595.8 potential years of life lost per 100,000 females, significantly fewer than for males and similar to figures reported for 2014. On average, each child or young person who died from avoidable causes lost 72 years of potential life.
Back to table of contents15. What has changed in this release?
Last year we revised our definition of avoidable mortality and developed an avoidable mortality definition for children and young people. Further information about the changes to the definition can be found on the consultation page of our website. Briefly, we found that:
there was an increase in the overall number of avoidable deaths in England and Wales under the revised definition of avoidable mortality compared with the previous definition; despite this increase, the age-standardised overall avoidable mortality rates under both definitions were not significantly different
there was a substantial increase in the number of deaths and age-standardised mortality rate for amenable (treatable) mortality in England and Wales; this was due to the classification of chronic obstructive pulmonary disease (COPD) as amenable to healthcare
because COPD is included in the previous definition of preventable mortality, its inclusion in the amenable mortality definition has no impact on the overall avoidable mortality figures
there was a small increase in the number of deaths from preventable causes under the new definition; despite this increase, the age-standardised preventable mortality rates under both definitions were not significantly different
The revised definition will be used to produce avoidable mortality indicators from data year 2014 onwards. We have not rebased previously published data on the revised definition, so this bulletin presents data for 2014 and 2015 only.
We will continue to review the avoidable mortality cause list and the associated age limits periodically. This means that any cause of death that has been excluded from the current list due to concerns around the extent to which deaths from it can be avoided will be reassessed and may be included in future lists.
Back to table of contents16. Concept of avoidable mortality
The concept of avoidable mortality was first introduced by Rutstein and others in the 1970s. Rutstein argued that, in order to develop effective indicators of healthcare, lists of diseases that should not (or only infrequently) give rise to death or disability should be drawn up (Rutstein and others, 1976).
Rutstein also noted that the list of conditions considered to be avoidable would need to be updated in light of improvements in medical knowledge and practice, as well as social and environmental changes. Although avoidable mortality has been researched for the last 3 decades, there is little consensus among researchers about how to define it.
The list of causes of death we used in defining avoidable mortality is primarily based on the cause lists produced by Nolte and McKee (2004) (PDF download) and Page, Tobias and Glover (2006) (PDF download). These cause lists were updated and amended to make them more relevant to the UK and to take account of more recent developments in healthcare public health policy. Changes to these lists were influenced by Wheller and others (2007), AMIEHS (2011) and views of respondents to the 2011 and 2015 consultations.
Statistics on avoidable mortality are used by central government, public health observatories, academia and charitable organisations working to reduce the prevalence of specific diseases and conditions deemed to be avoidable causes of death.
One of the main expected uses of these statistics is the monitoring of the quality performance of healthcare and public health policies. The Department of Health uses potential years of life lost (PYLL) from causes considered amenable to healthcare for children and young population in its NHS Outcomes Framework 2016/17 (Department of Health, 2016) and mortality from preventable causes as an indicator in its Public Health Outcomes Framework to reduce preventable ill-health, population dying prematurely and to reduce the gap between communities (Department of Health, 2015).
Further information on avoidable mortality indicators used at international level is available in the avoidable mortality quality and methodology information notes.
Back to table of contents17. References
AMIEHS (2011) Avoidable mortality in the European Union: Towards better indicators for the effectiveness of health systems, Final Report (viewed on 17 June 2016)
Department of Health (2015) NHS Outcomes Framework 2016/17 (viewed on 17 June 2016)
Department of Health (2014) Public Health Outcomes Framework (viewed on 17 June 2016)
Nadkarn S, Cooper D, Brancaleone V, Bena S and Perretti M (2011) Activation of the Annexin A1 pathway underlies the protective effects exerted by estrogen in polymorphonuclear leukocytes: Arteriosclerosis, Thrombosis and Vascular Biology (viewed on 17 March 2017)
Nolte E and McKee M (2004) Does health care save lives? Avoidable mortality revisited. The Nuffield Trust, London (viewed on 17 June 2016) (PDF download)
Office for National Statistics (2016a) Deaths registered in England and Wales (Series DR): 2015 (viewed on 15 March 2017)
Office for National Statistics (2016b) Provisional analysis of deaths registrations: 2015 (viewed on 17 March 2017)
Office for National Statistics (2016c) Revised Definition of Avoidable Mortality and New Definition for Children and Young People (PDF download)
Page A, Tobias M, Glover J, Wright C, Hetzel D and Fisher E (2006) Australian and New Zealand Atlas of Avoidable Mortality, University of Adelaide: Adelaide: Public Health Information Development Unit (viewed on 11 May 2016)
Rutstein DD, Berenberg W, Chalmers TC, Child CG, Fishman AP, Perrin EB, Feldman JJ, Leaverton PE, Lane MJ, Sencer DJ, and Evans CC (1976). Measuring the quality of medical care - A clinical method. New England Journal of Medicine 294: 582–588 (viewed on 11 May 2016)
Wheller L, Baker A, Griffiths C, Rooney C (2007). Trends in avoidable mortality in England and Wales. Health Statistics Quarterly, 34, 6–25 (viewed on 11 May 2016) (PDF download)
Back to table of contents18. Upcoming changes to this bulletin
We plan to release a follow-up article before the next release of this bulletin. The article will report on the inequality in avoidable, amenable and preventable mortality using measures of area-based deprivation in England and Wales separately. We plan to incorporate analyses of the inequality in these measures into future releases of this bulletin.
Back to table of contents19. Data requests
Special extracts and tabulations of avoidable mortality (and other causes of mortality) data for England and Wales are available to order for a charge (subject to legal frameworks, disclosure control, resources and agreement of costs, where appropriate). Such requests or enquiries should be made to:
Mortality Analysis Team, Life Events and Population Sources Division
Office for National Statistics
Government Buildings
Cardiff Road
Newport
South Wales NP10 8XG
Tel: +44 (0)1633 456736
Email: mortality@ons.gov.uk.
Our charging policy is available on our website.
Back to table of contents20. Quality and methodology
The Avoidable mortality Quality and Methodology Information document contains important information on:
- the strengths and limitations of the data and how it compares with related data
- uses and users of the data
- how the output was created
- the quality of the output including the accuracy of the data
Age-standardised rates were calculated using the number of potentially avoidable deaths registered in each year as the numerator and the mid-year population estimate for that year as the denominator.
Although age limits were set for some cause groups, rates were calculated using people of all ages as the denominator to allow data by cause group, amenable and preventable categories to be presented on a comparable basis. For the children and young people’s indicator, an upper age limit of 19 years was used to calculate age-standardised rates.
Potential years of life lost (PYLL) is a measure of the potential number of years lost when people die prematurely from any cause. The basic concept underpinning PYLL is that deaths at younger ages are weighted more heavily than those at older ages. The advantage in doing this is that deaths at younger ages may be perceived to be of less importance if cause-specific death rates alone were used to highlight the burden of disease and injury, as conditions such as cancer and heart disease often occur at older ages and have relatively high mortality rates.
To enhance comparability between areas and the sexes, we have standardised PYLLs using the 2013 European Standard Population (ESP). It is therefore referred to as standardised years of life lost (SYLL) for clarity. SYLL rates represent the potential years of life lost if the population of England and Wales had the same population structure as the 2013 ESP. The rates are presented as years of life lost per 100,000 population. Detailed explanations on how this indicator is calculated are available in the Avoidable mortality Quality and Methodology Information notes.
The average years of life lost (AYLL) is a measure of the potential number of years lost when an individual dies prematurely from any cause. It is calculated by summing up the number of deaths in each age group, weighted by the corresponding remaining life expectancy and then dividing the result by the total number of deaths across all age group.
Statistics on mortality are derived from the information provided when deaths are certified and registered. Further information about the methods and quality of these statistics can be found in the Quality and Methodology Information. We hold mortality data for England and Wales. Figures for the UK include data kindly provided by National Records of Scotland and the Northern Ireland Statistics and Research Agency.
Differences referred to in this bulletin are based on unrounded figures. A difference that is described as “statistically significant” has been assessed using 95% confidence intervals. If a difference is said to be statistically significant, it is unlikely that it could have occurred by chance alone. Confidence intervals give a measure of the statistical precision of an estimate and show the range of uncertainty around the estimated figure. As a general rule, if the confidence interval around an estimate overlaps with the interval around another, there is no significant difference between the two estimates. When the number of deaths is less than 100, the method used to calculate confidence intervals is different (see Dobson et al., 1991).
